Yo Kishimoto, M.D., Ph.D.
Associate Professor,
Department of Otolaryngology-Head and Neck Surgery,
Graduate School of Medicine, Kyoto University, Kyoto, Japan
1. Importance of Endoscopic Examination in Head and Neck Practice
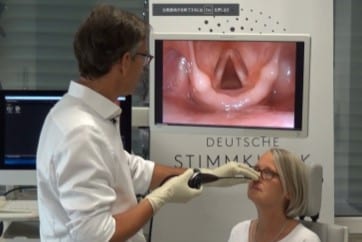
Endoscopic examination plays a central role in head and neck practice, with white-light imaging serving as the fundamental modality. Using white-light observation, most elevated lesions, including vocal fold polyps, can be accurately diagnosed. Recent technological advances have markedly improved image quality, enabling more detailed observation and enhanced diagnostic performance. Furthermore, the ability to digitally record endoscopic findings has made endoscopy an indispensable diagnostic tool in contemporary head and neck practice.
However, the early detection of superficial laryngopharyngeal car cinoma, which has been increasing in recent years, remains challenging with white-light observation alone. In addition, evaluation of vocal fold vibration in voice disorders and assessment of tumor depth in glottic carcinoma are not possible using white-light imaging alone. These evaluations become feasible only through narrow band imaging (NBI) and stroboscopic observation, respectively. Such highprecision diagnostic modalities are clinically essential, as they directly contribute to appropriate treatment selection and improved therapeutic outcomes.
With conventional otolaryngologic endoscopes, NBI observation has often been limited by lower resolution compared with gastrointestinal endoscopes and by frequent halation due to surface reflection, which can complicate diagnosis. Similarly, stroboscopic observation has frequently suffered from insufficient illumination, making accurate assessment of mucosal vibration difficult, particularly in patients with strong reflectivity where close observation is challenging.
Moreover, when NBI for microvascular assessment and stroboscopy for depth evaluation are used in combination for the diagnosis of early glottic carcinoma, switching between different light sources is required, resulting in procedural complexity for both healthcare providers and patients.
2. Features of VISERA S OTV-S500
VISERA S OTV-S500 is a light-source-integrated endoscopic system that enables the use of a stroboscopic observation mode through software upgrades via a portable memory port. This system eliminates the need to change light sources and allows seamless, one-touch switching between NBI and stroboscopic observation.
Functionally, the system employs narrow-spectrum violet LEDs in addition to white LEDs, thereby enhancing image contrast during NBI observation. Noise reduction is achieved through frame accumulation and image processing techniques. Furthermore, increased luminous intensity enabled by high-current output, combined with the integrated light-source design, allows advanced in-system image processing. This configuration suppresses flicker caused by mismatches between the camera shutter speed and the light source flashing cycle.
Another notable feature of the system is its compact and lightweight design. The main unit measures 308 mm in width, 157 mm in height, and 461 mm in depth, with a total weight of only 10.6 kg, facilitating easy transportation and installation in operating rooms and other clinical settings.
3. Clinical Utility of VISERA S OTV-S500 in Early Detection and Extent Assessment of Superficial Head and Neck Cancer and High-Gr ade Dysplasia
Case 1: Oropharyngeal Squamous Cell Carcinoma (cT1N0M0)
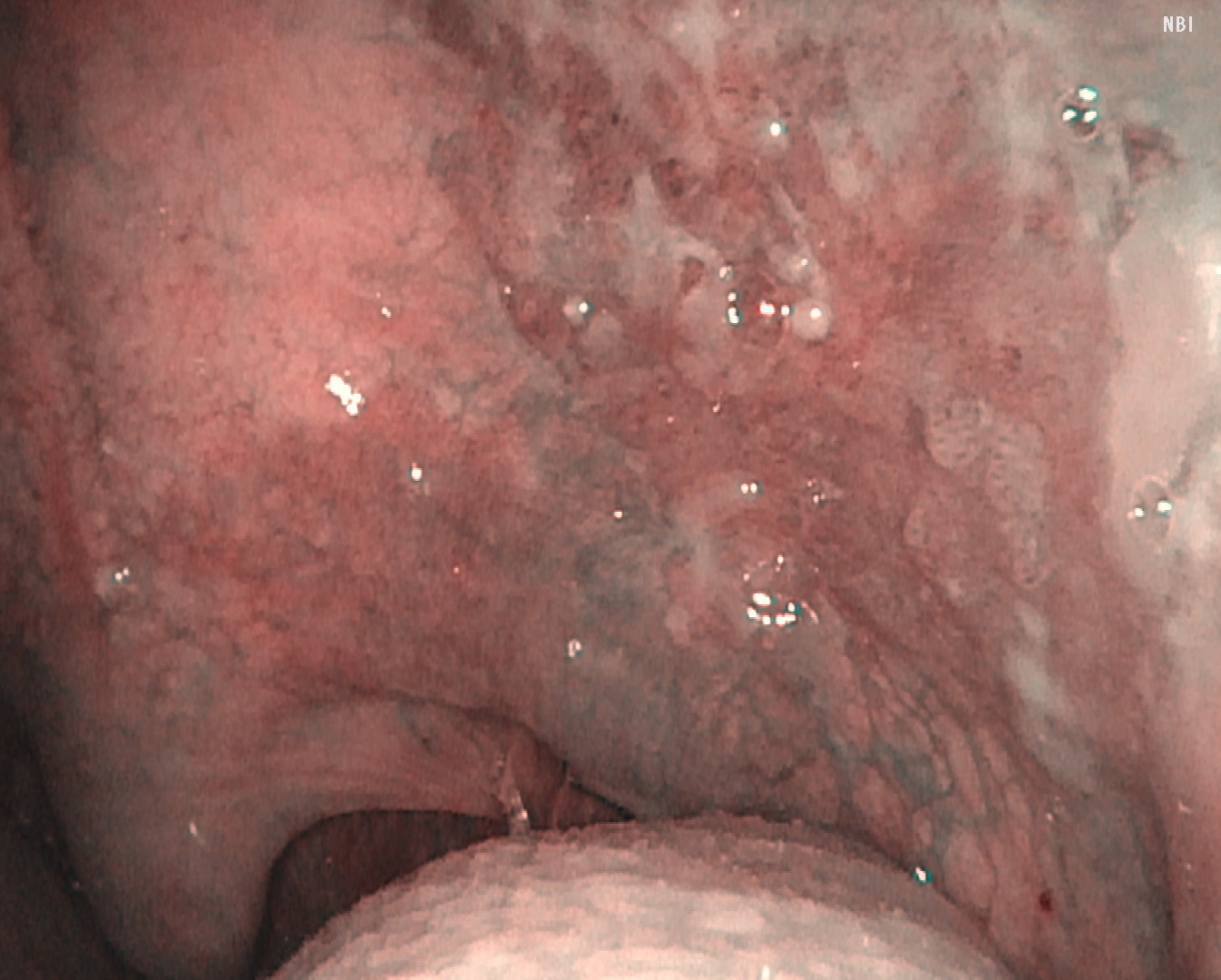
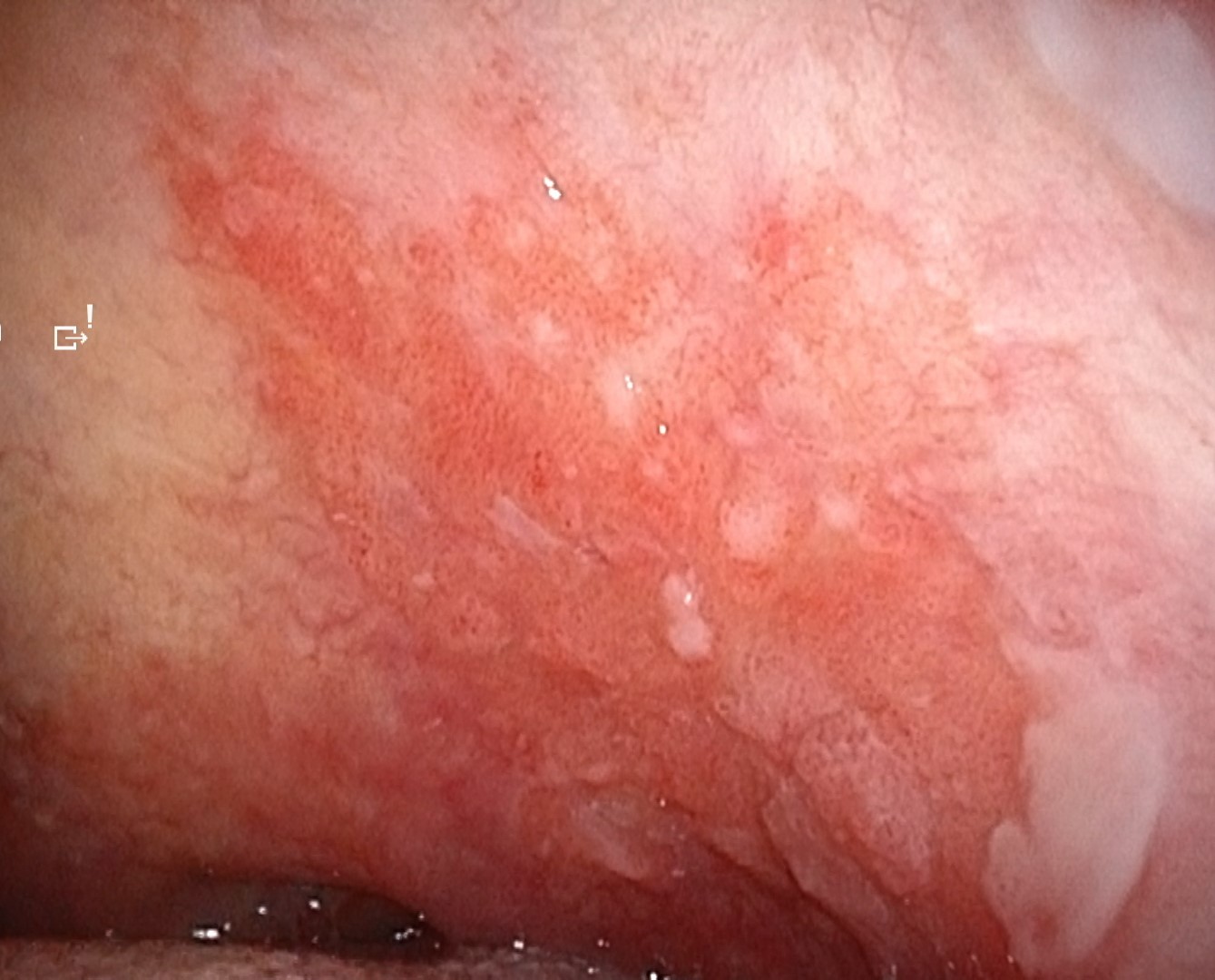
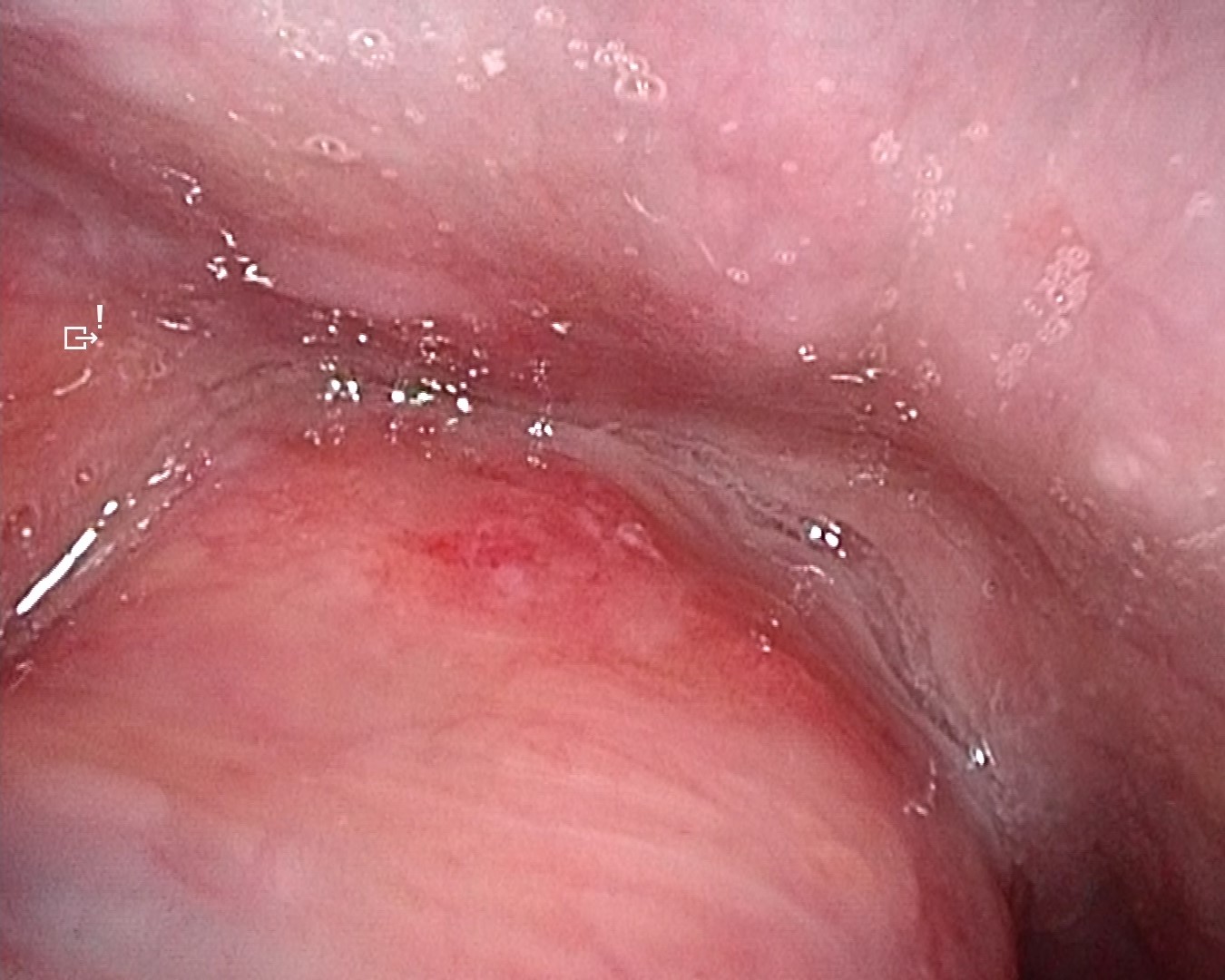
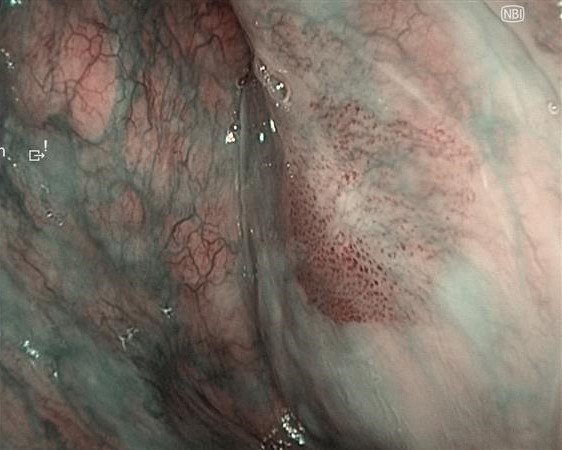
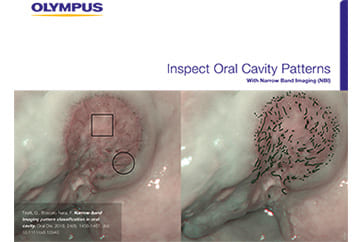
White-light observation revealed an erythematous lesion with an irregular surface extending from the left soft palate to the anterior palatine arch; however, accurate assessment of lesion extent was difficult. NBI observation demonstrated a well-demarcated brownish area with proliferative atypical microvessels. Compared with conventional systems (OTV-S190), VISERA S OTV-S500 provided enhanced contrast, allowing clearer delineation of tumor extension.
Case 2: Hypopharyngeal High-Grade Dysplasia
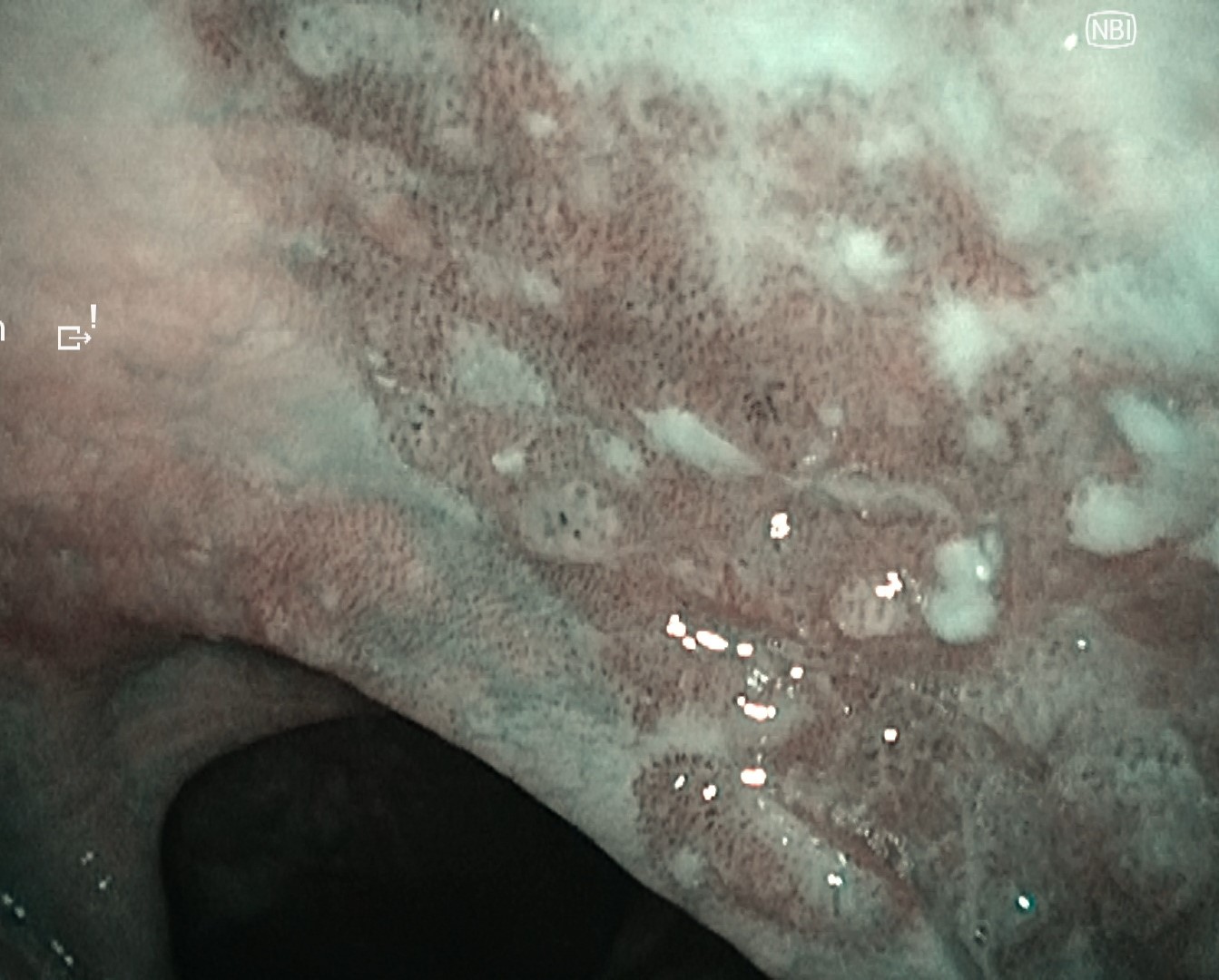
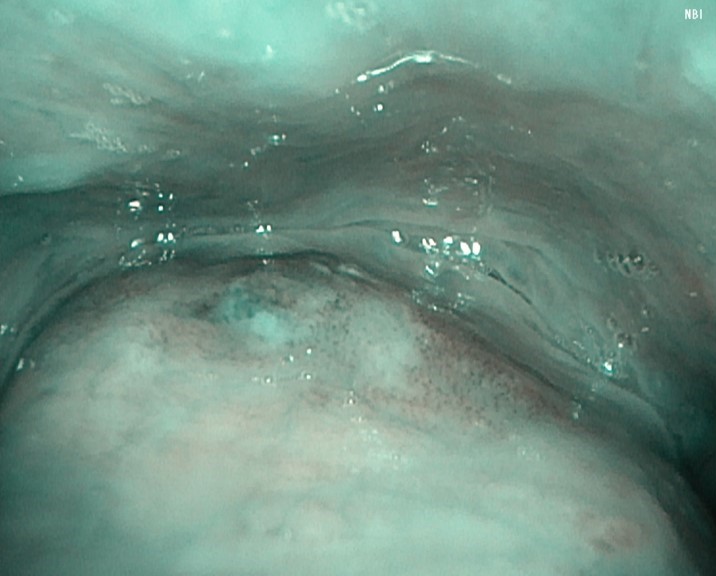
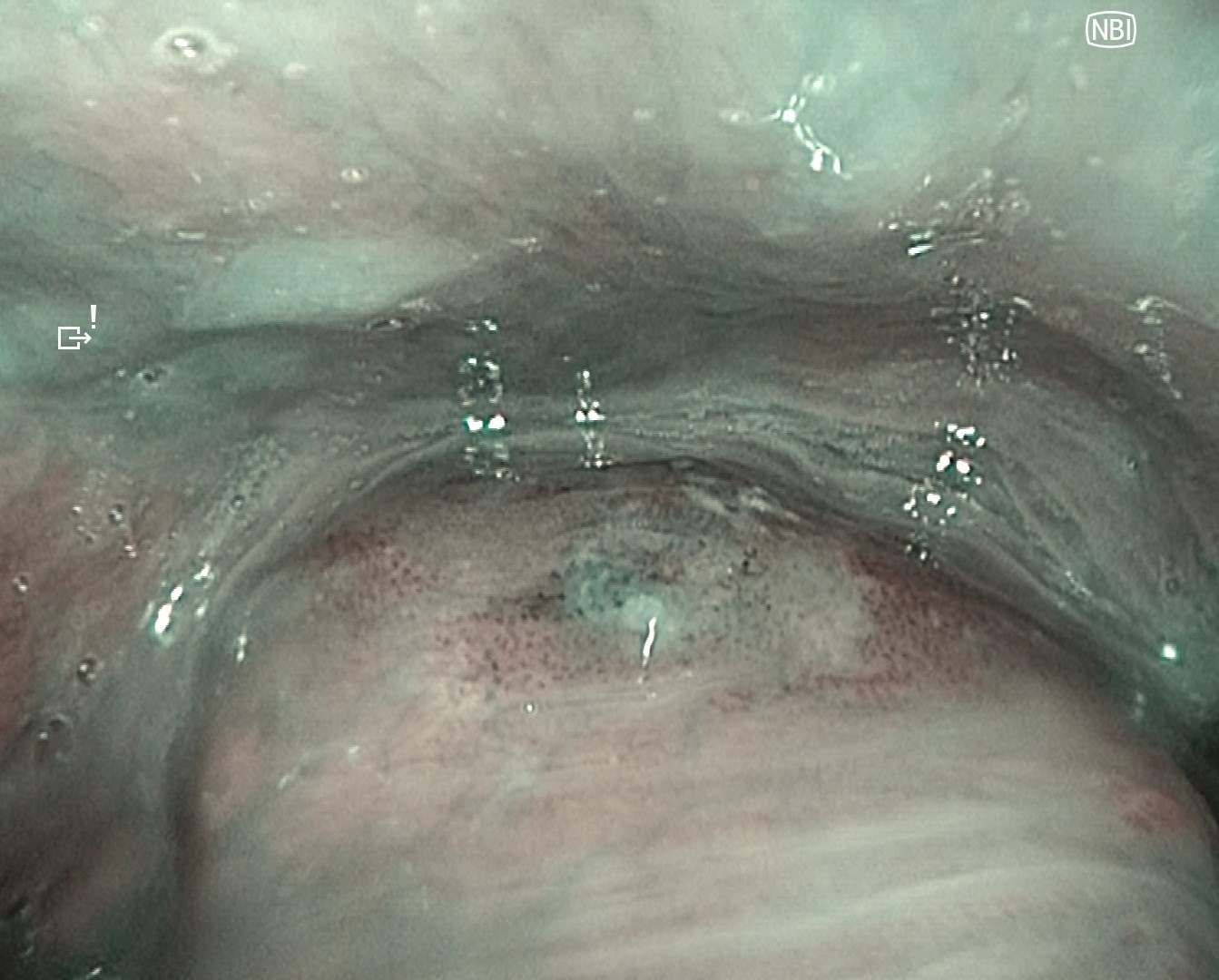
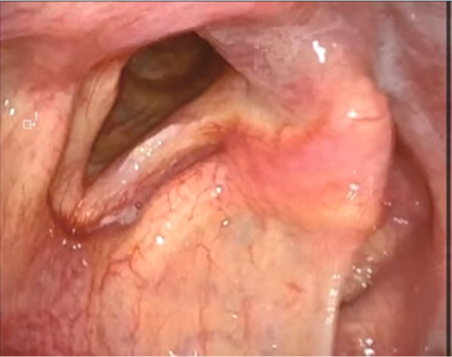
Following observation of the hypopharynx using the modified Killian m ethod, slight erythema was noted on the mucosa of the right pyriform sinus. NBI observation revealed a clearly demarcated brownish area with atypical microvascular proliferation at the same site. Compared with VISERA ELITE OTV-S190, VISERA S OTV-S500 provided stronger contrast and improved lesion visibility.
Case 3: Hypopharyngeal High-Grade Dysplasia
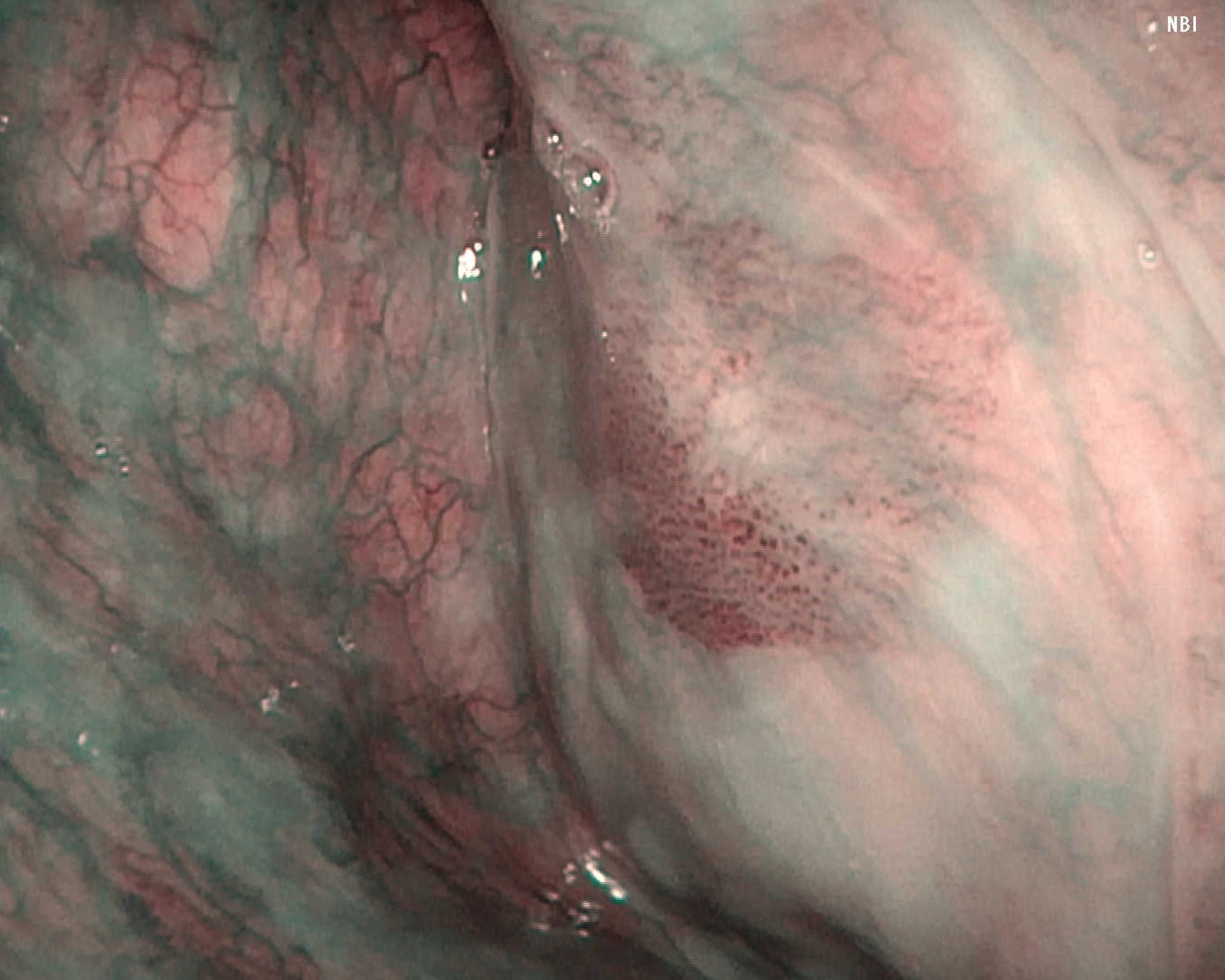
Under general anesthesia, the left pyriform sinus was observed after hypopharyngeal exposure. A well-defined brownish area with atypical microvessels was identified.
Compared with VISERA ELITE OTV-S190, VISERA S OTV-S500 demonstrated reduced color and luminance unevenness due to noise reduction processing, improved depth of field, and sharper edge definition, resulting in clearer visualization of the lesion.
Case 4: Vocal Fold Carcinoma in Situ
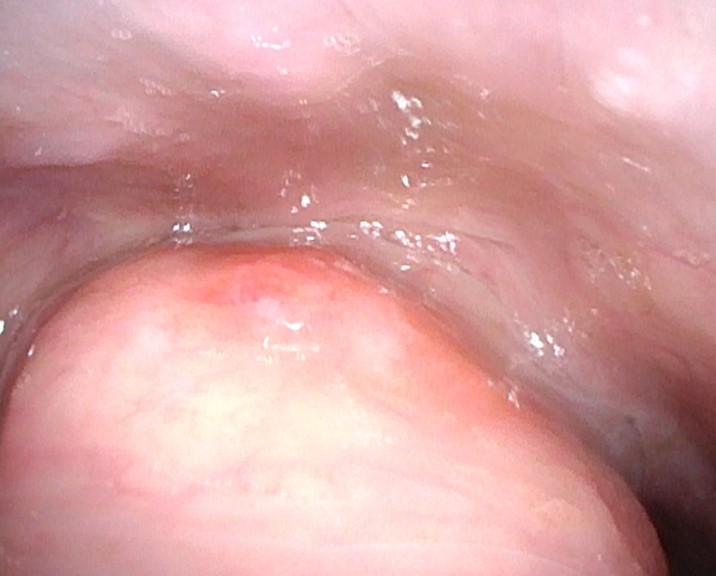
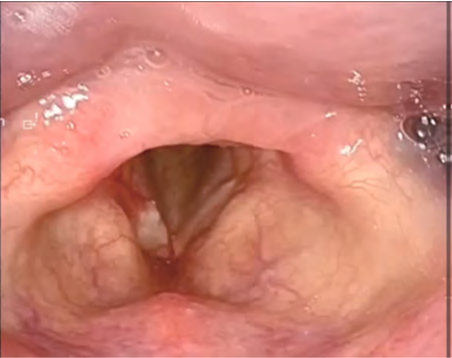
A thin whitish lesion was observed on the vocal fold. No extension to the anterior commissure was noted, and NBI observation revealed no surrounding atypical vessels. Stroboscopic examination demonstrated relatively preserved mucosal wave motion, suggesting the absence of deep tissue invasion.
Case 5: Spindle Cell Squamous Cell Carcinoma of the Right Vocal Fold
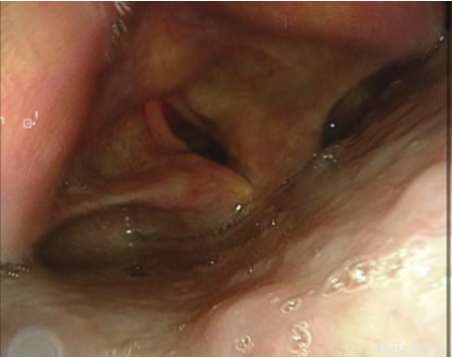
A white, elevated lesion was observed on the right vocal fold. NBI observation revealed clustered vascular structures posterior to the white lesion; however, no surrounding brownish area or atypical vessels were observed, and no extension to the anterior commissure was identified. Stroboscopic examination showed reduced mucosal wave motion of the right vocal fold, suggesting the presence of malignancy and possible invasion into the vocal ligament. During sustained phonation, supraglottic constriction was also observed.
Case 6: Left Vocal Fold Paralysis
A patient with left vocal fold paralysis caused by esophageal cancer invasion underwent type I thyroplasty and arytenoid adduction under local anesthesia. Intraoperative stroboscopic observation enabled confirmation of medialization of t he vocal fold and mucosal vibration. Adjustment of the degree of medialization altered the symmetry and regularity of mucosal vibration, and the maximum phonation time was ultimately prolonged from 4.6 seconds to approximately 20 seconds.
Conclusion
In the light-source-integrated VISERA S OTV-S500 system, enhanced image processing performance has led to substantial improvements in imaging capability. In addition to conventional white-light observation, the system provides high-contrast NBI using violet LEDs and stroboscopic observation with sufficient illumination, both of which can be switched seamlessly with a single operation. These features contribute to early detection of malignant lesions, accurate assessment of tumor extent, and detailed evaluation of vocal fold mucosal vibration.
By appropriately utilizing the characteristics of this system, improvements in diagnostic accuracy and examination efficiency can be achieved, offering significant benefits for both patients and healthcar e providers. VISERA S OTV-S500 is therefore considered a valuable system that enhances the quality of endoscopic diagnosis in head and
neck practice, supporting a wide range of applications from routine clinical care to advanced diagnostic evaluation.
Disclaimer
The techniques and clinical opinions presented in this material reflect the personal experience and professional judgment of the healthcare professional and do not necessarily represent the views of Olympus. This material is intended for healthcare professionals only. This material is not intended to substitute the Instructions for Use (IFU). Users should always refer to the applicable IFU and use Olympus products in accordance with the approved indications and local regulatory requirements. The healthcare professional presenting this material has been engaged by Olympus and compensated at fair market value for their services.
- Content Type