Tips on ITknife nano usage by
a needle-type ESD knife user
– Aiming at safe, efficient esophageal/colorectal ESD –
Professor of Gastrointestinal Endoscopy, Tokyo Women’s Medical University Hospital
Biography
Graduated from Shimane Medical University (presently Shimane University Medical School) in 2002. After training at Kumamoto University Hospital and several other institutions, Dr. Nonaka became a professor in the Department of Gastrointestinal Endoscopy at Tokyo Women’s Medical University. Dr. Nonaka has for many years been actively mentoring young endoscopists in diagnosis and therapy not only in Japan, but throughout Asia as well. In April 2024 he received an award from the Vietnamese Federation for Digestive Endoscopy for many years of endoscopy training in Vietnam. His textbooks for diagnosis of gastrointestinal endoscopy have been translated and widely distributed in four Asian countries.
Since the advent of the Helicobacter pylori-negative era, ESD for early gastric cancer has declined significantly. In contrast, colorectal ESD has been increasing, while the rate of esophageal cases has remained quite stable. These procedures are more technically demanding than gastric ESD and require considerable skill. Many hospitals now use needle-type knives such as the DualKnife. Ideally, a single knife would suffice, but for esophageal and colorectal ESD a second device is often advisable to reduce technical difficulty and complications. It has been more than two decades since ESD was introduced, and in that time several traction methods devised to improve safety have become mainstream. I use clip-with-line traction in almost all esophageal cases and in 70 – 80 % of colorectal cases, achieving a risk-minimized ESD with optimal promptness. For procedures in this traction era, the use of the ITknife nano as a second device has been found helpful in my own experience.
Features of ITknife nano
Currently, needle-type knives have become the mainstream, and the standard approach in ESD is to advance by pushing and cutting in the direction toward the lumen during mucosal incision and submucosal dissection. The ITknife, in contrast, is operated in precisely the opposite way – that is, you pull the knife towards you, rather than advancing it.
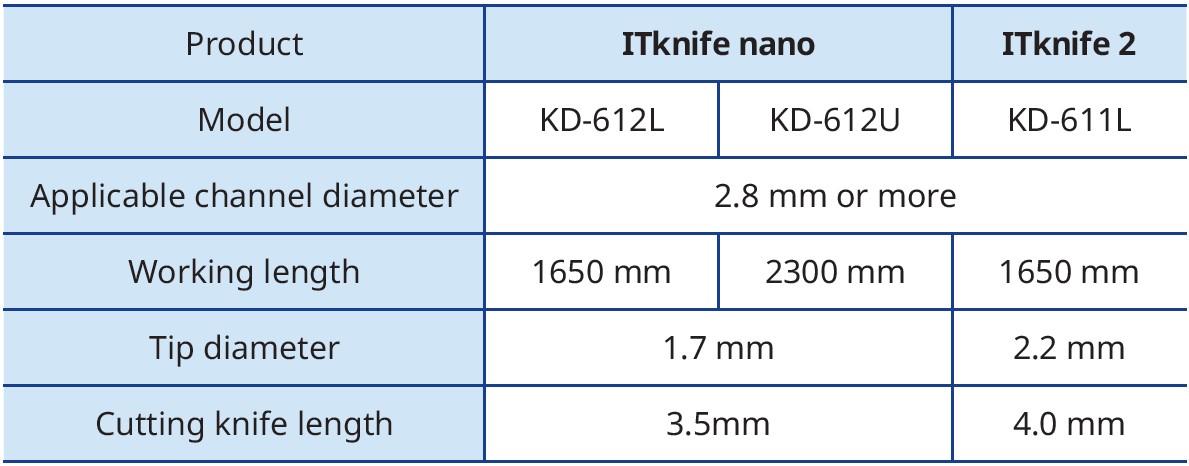
For operators unfamiliar with the ITknife, mastering a very sharp knife such as the ITknife 2 – which features three electrodes on the back of its insulated tip – can be daunting.
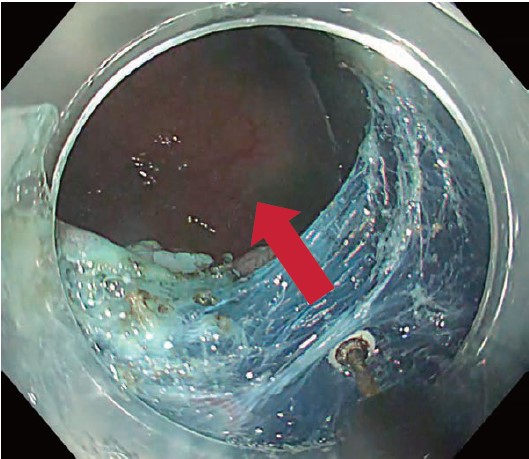
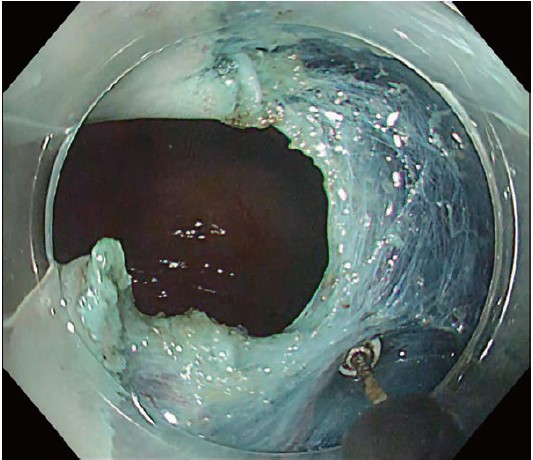
Compared with the ITknife 2, the ITknife nano is “not excessively sharp” and has a smaller insulated tip (Figs. 1 & 2).
Perhaps the greatest advantage of the ITknife nano is that it is “not excessively sharp”. When combined with a small insulated tip, this less-aggressive blade means that the ITknife nano is much easier to master, making it an ideal second device for risk-minimized esophageal and colorectal ESD. As a dedicated needle-type knife user and frequent DualKnife user, I would like to share tips for exploiting these features, as well as for combining the ITknife nano with traction techniques for a riskminimized and time-efficient ESD.
ITknife nano in esophageal ESD
The esophagus is a straight lumen, so why is ESD so difficult? Despite the fact that it is straight, the view inside the esophagus can be easily shifted by a variety of factors including the heartbeat, respiratory vibrations, hiccups, and body movements. One slip could lead to perforation – a potentially fatal complication. This is where the ITknife nano’s insulated, not so sharp tip comes into its own; the assistant need only push or pull the knife.
Because perforation is unlikely unless substantial pressure is applied directly to the muscularis, the ITknife nano improves safety. Its relatively stiff sheath and small tip also let the operator lift the lesion and confirm the dissection plane.
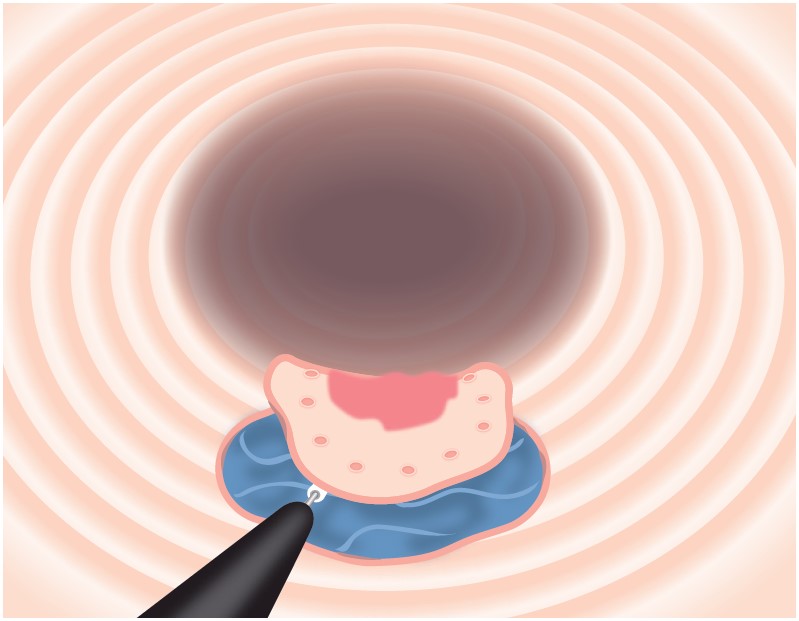
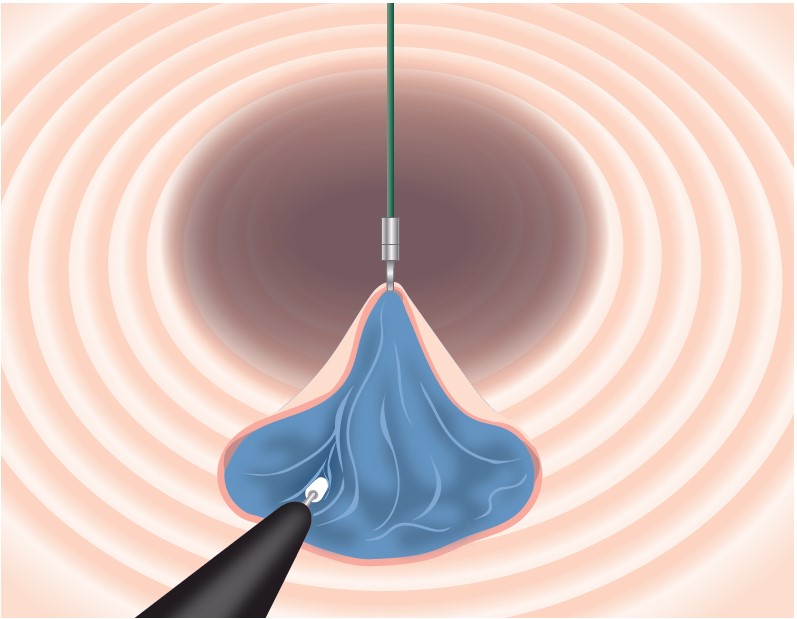
However, this added safety can decouple knife motion from dissection speed, tending to shallow the dissection layer (Fig. 3). Traction solves this completely. Clip-with-line traction stands the submucosa upright – like the adductor muscle of a scallop – enabling efficient, rapid dissection with the 3.5-mm blade while preserving the safety benefits of the ITknife nano tip and the safety of the “not excessively sharp” blade (Fig. 4).
If patient movement or hiccups slow the procedure, I immediately use the ITknife nano with thread traction; the case can still be finished quickly while exploiting the knife’s safety.
Although the tip is insulated, incorrect angle or excessive pressure can still damage the muscle – a concern that has slowed adoption among some users. I therefore recommend “push-cut mucosal incision”. The smaller tip of ITknife nano fits easily into narrow submucosal spaces, allowing a riskminimized, deliberate incision by pushing – almost the same feel as with conventional knives, yet with the benefit of insulation.
Do not get caught up in the idea that you must always pull the ITknife for cutting; combine pushing and pulling as the situation demands.
ITknife nano in colorectal ESD
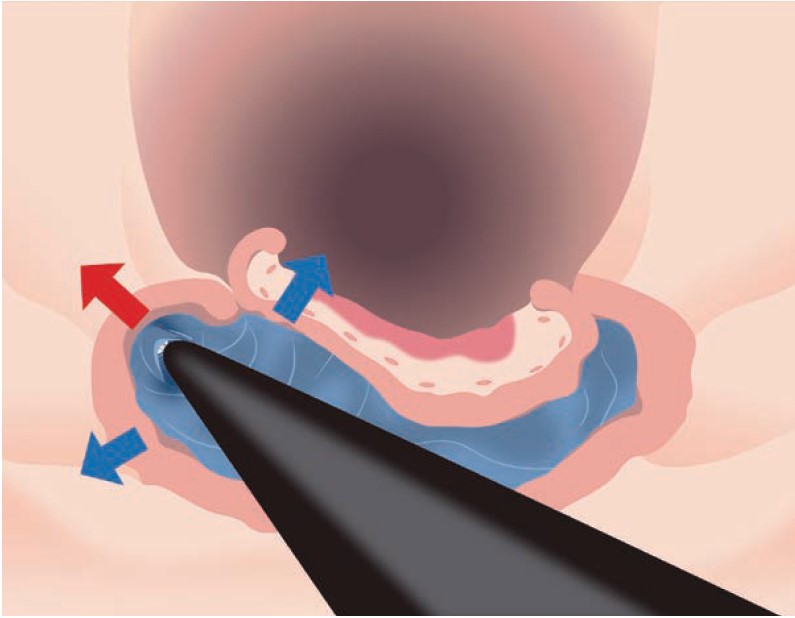
Because of the colon’s curves and folds, unseen muscularis may lie in the knife path; pull-cutting can cause perforation, so it is usually avoided. Depending on scope position, pulling the ITknife from the five- or seven-o’clock channel can damage an unexpected fold, which understandably makes users hesitant. So why not dissect by pushing instead? As in the esophagus, the compact insulated tip allows the knife to crawl into the submucosa and dissect “from inside to outside”, i.e., toward the lumen, just like other knives – virtually eliminating perforation risk (Fig. 5). Efficient dissection with the blunt 3.5-mm blade and the ITknife nano safety profile is possible when the submucosa is kept upright with traction. Even in the transverse colon, where the effects of respiratory vibration are pronounced, or in the cecum, where the muscle runs perpendicular, the insulated tip makes perforation unlikely unless very strong force is applied. Lightly brushing the insulated tip on the muscle can actually stabilize the scope and shorten dissection time.
High-frequency settings for ITknife nano
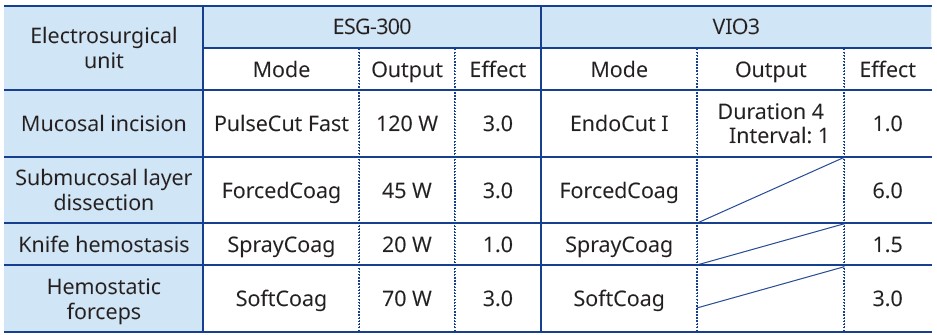
Before presenting actual cases, suggested electrosurgical unit settings are shown in Fig. 6. Because the ITknife nano is longer than the DualKnife, current density can fall during tissue cutting. When using ITknife nano, dissecting the submucosal layer is generally easier in a coagulation wave – such as ForcedCoag – than in a pure cutting wave, owing to the higher peak voltage of the former.
Presentation of esophageal case (1)
The following are actual cases in which I used the ITknife nano. The first case was a small 0-IIa lesion on the left side of the midthoracic esophagus.
Mucosal incision and flap creation were begun with a DualKnife. When cardiac pulsation, respiratory motion, or hiccups hampered precise cutting, switching to ITknife nano provided a steadier tactile sense. For extremely fine lateral incisions which require adjustments on the order of millimeters to preserve the normal mucosal, the ITknife nano is not appropriate (as shown in the video) and the DualKnife remains preferable.
Once the flap was raised, clip-with-line traction was applied, and submucosal dissection was completed fairly quickly with the ITknife nano (Fig. 7, Movie 1). With traction in place, the theoretical risk of perforation approaches zero. Dissection is performed in coagulation mode, melting the tissue while keeping the white insulated back of the tip visible through the blue submucosa (Fig. 8).
Safety is enhanced by pushing the knife toward the lumen rather than pulling proximally.
Pull-cutting often slows the operator and leads to a shallow plane because of fear of damaging the muscle layer. Pushing the ITknife nano forward instead can produce surprisingly rapid
progress, the blunt tip tunnelling through the submucosa while maintaining a generous safety cushion.
In the author’s experience, combining clip-with-line traction with ITknife nano provides the greatest safety and confidence during esophageal ESD.
Movie 1 Esophageal case (1)
Presentation of esophageal case (2)
This case involved a 0-IIc lesion on the posterior wall of the mid thoracic esophagus, adjacent to a post ESD scar. Submucosal lifting was insufficient despite hyaluronic-acid injection (Figs. 9 & 10). Using an ultra-sharp DualKnife in this situation carries a measurable perforation risk and increases operator anxiety. Instead, a “push-through mucosal incision” with the small insulated tip of ITknife nano was chosen (Movie 2).
After lifting on the oral side of the scar, the tip was advanced and a blunt, controlled mucosal cut was made (Figs. 11 & 12). Once a full circumferential incision was complete, the remainder of the dissection was finished quickly and safely with the ITknife nano blade, achieving en-bloc resection in a short time.
Movie 2 Esophageal case (2)
Presentation of colorectal case
A 50 mm laterally spreading tumour in the ascending colon was addressed (Fig. 13). With ITknife nano the fundamental manoeuvre is “inside to outside”, advancing toward the lumen (Fig. 14).
Even when a large vessel or ambiguous fold obscured the plane, safe dissection was possible by first creating a small ‘hold’ on the vessel side – lightly melting the blue submucosa with the insulated tip – then continuing the inside to outside approach (Fig. 15, Movie 3).
Should gravity or scope instability slow progress, traction is applied to stand up the submucosa. Once the tissue is standing, rapid dissection can be performed with the ITknife nano without altering patient position, completing the resection efficiently.
Movie 3 Colorectal case
Conclusion
Twelve years after its launch, many young endoscopists begin ESD without appreciating the characteristics of the ITknife nano. As an needle-type knife user, I have shown how to perform risk-minimized ESD with the ITknife nano by simply “pushing” toward the lumen as with needle-type knives, and how well the knife pairs with traction techniques for risk-minimized and time-efficient procedures.

Location: Kawada-cho 8-1. Shinjuku-ku, Tokyo, Japan / Number of beds: 769 (as of 2024)
Founded in 1908, the hospital performs more than 8,000 operations annually across about 50 departments, including minimally invasive and robotic surgery. Since 2020, ESD volume has grown rapidly, with roughly 200 esophageal/gastric cases and about 250 colorectal cases per year.
- Keyword
- Content Type


.png)
.png)
.jpg)
.png)
.png)
.png)
.png)