Dr. Hirokazu Noshiro, Professor, Chairman of Department of Surgery,
Faculty of Medicine, Saga University
Biography
Graduated from Kyushu University, School of Medicine in 1985, and chairman of the Department of Surgery, Faculty of Medicine, Saga University in 2010. Since 2016, Vice President of Saga University Hospital. Known as an expert in cancer treatment of digestive organs, especially using endoscopic surgery for gastric and esophageal cancer, he was one of the first surgeons to introduce robotic surgery in Japan and is currently active in this field.
Characteristics of 4K Endoscope
The Olympus 4K endoscope used in the present case has about four times as many pixels as that of a full high-definition (HD) endoscope.
The 4K endoscope is characterized by enhanced “reality perception related to stereoscopic feeling” due to high pixel density similar to human vision, as well as clear depiction and shading with almost natural colors, resulting in the illusion of a three-dimensional effect arising from the planar image in the brain. In the Olympus 4K endoscope system, the entire imaging chain including the system, optics, camera head, monitor and recorder has been optimized for 4K aiming at the best performance of the 4K endoscope. Three major characteristics of the 4K endoscope are: 1. high-definition, 2. wide-color gamut and 3. magnified visualization by the use of widescreen monitor and electronic zoom. For example, in developing an optics exclusive for 4K, a special low-dispersion lens for single-lens reflex cameras has been used, realizing the clear and sharp image visualization without color bleeding. In the present report, the clinical usability of these characteristics of the 4K endoscope for thoracoscopic esophagectomy in the prone position was evaluated.
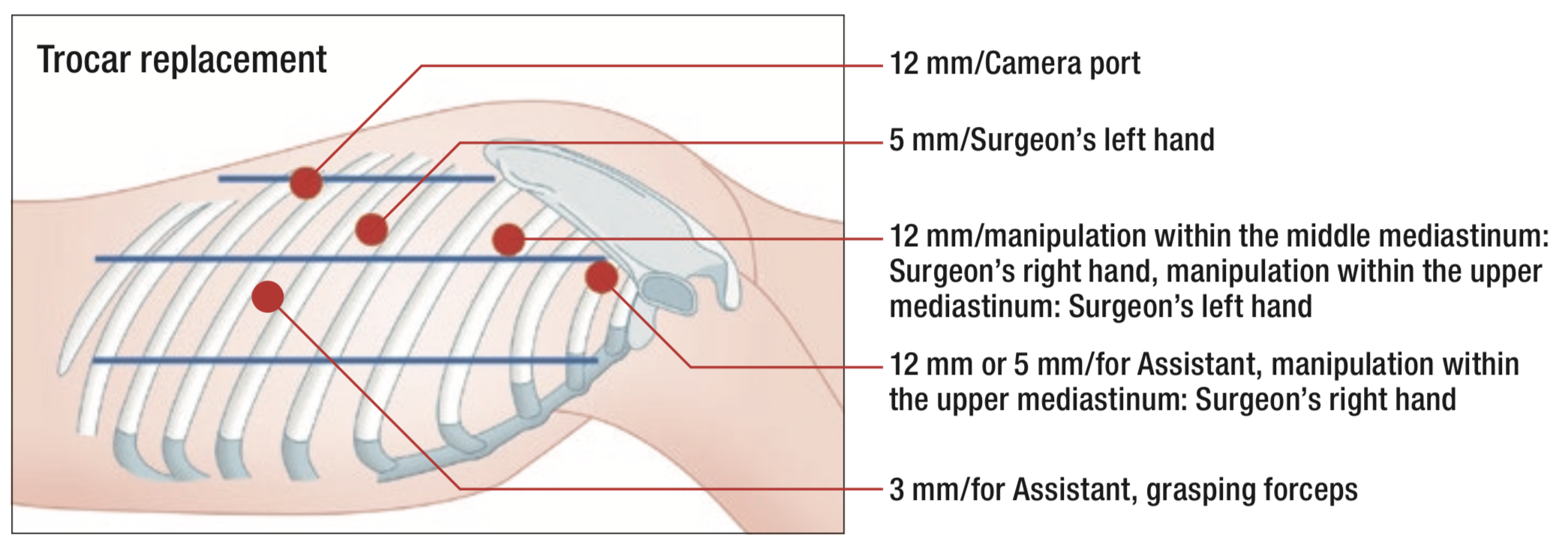
Procedures of Thoracoscopic Esophagectomy in the Prone Position
Thoracoscopic surgery in the prone position was introduced at our institute in December 2007 as a thoracic procedure during radical surgery for thoracic esophageal carcinoma. It has since been developed as standard due to its minimal invasiveness. Endoscopic systems provided easy identification of microanatomy under magnification and thus allowed surgeons to preserve vessels and nerves, as well as perform complete mediastinal lymphadenectomy with the better surgical fields. Thoracoscopic surgery in the prone position, which was considered easier to manage, was expected to preserve postoperative respiratory function and reduce postoperative pulmonary complications by minimizing damage to the body wall.
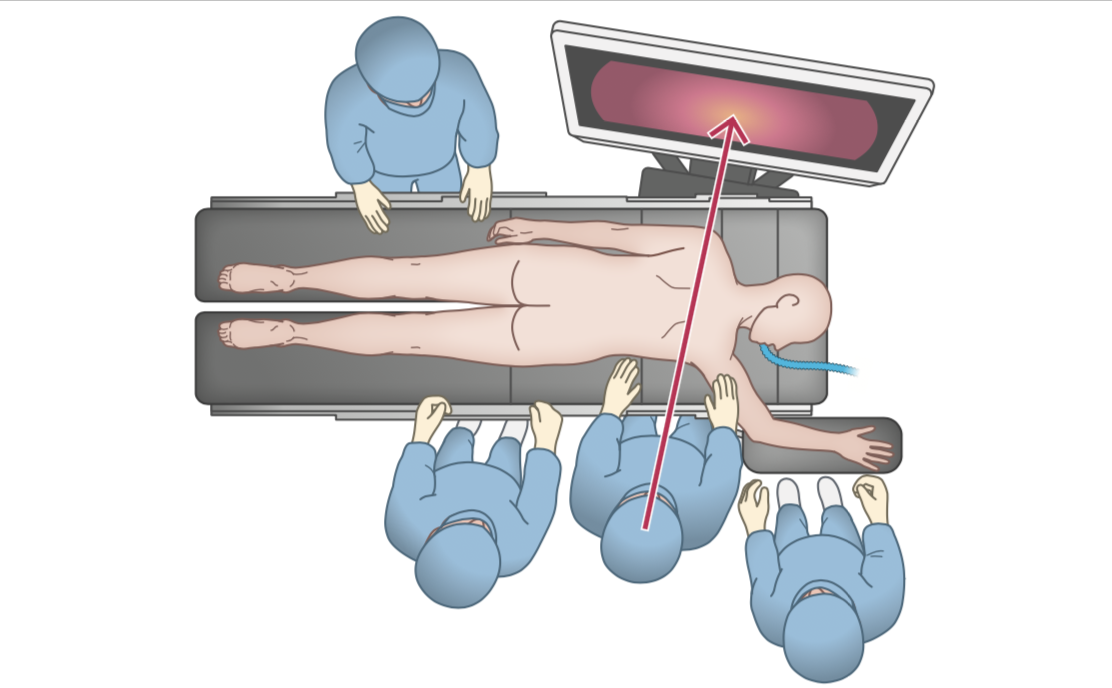
All surgeons, including the first assistant and the camera holder, stood on the right side of the prone patient and looked at the 4K/55-inch monitor screen on the opposite side. The 4K/55-inch monitor could display magnified high-definition images from the 4K endoscope. This magnification and clarity provided a sense of visual realism.
Clinical Usability of the 4K System in Thoracoscopic Esophagectomy in the Prone Position
1. From cutting the pleura to dividing the arch of azygos vein
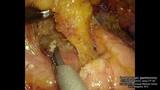
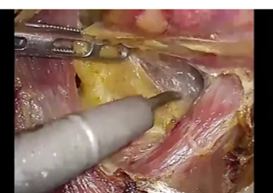
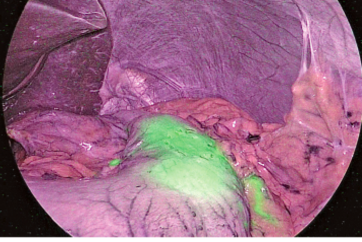
For the posterior mediastinum, the operating table was rotated to slightly elevate the right side, and the mediastinal pleura was cut along the azygos vein. During this procedure, the dissectible layer between the thoracic duct and the surrounding fat was further emphasized by the wide color gamut of the 4K endoscope compared to the full HD endoscope. This distinction was very important to dissect the lymph nodes while preserving the thoracic duct. After ligating and clipping, the azygos arch was divided using the THUNDERBEAT™ device. To better expand the visual field in the posterior upper mediastinum, the dorsal stump of the divided azygos arch was fixed to the back side. Suturing, if requested, could also be performed safely and easily, because the needle and thread could be visualized stereoscopically due to the stereoscopic visual effect provided by the 4K endoscope.
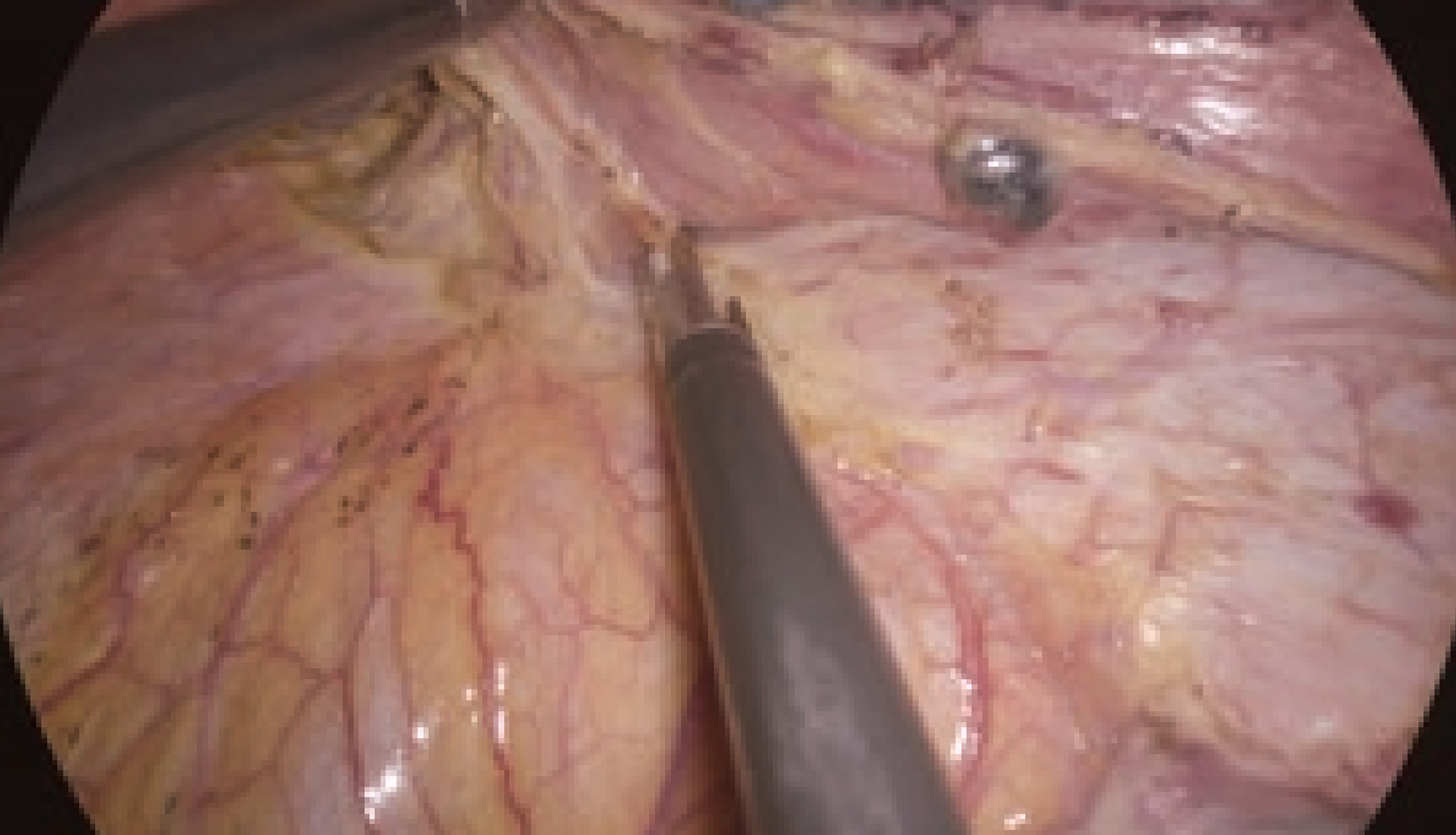
(wide color gamut)
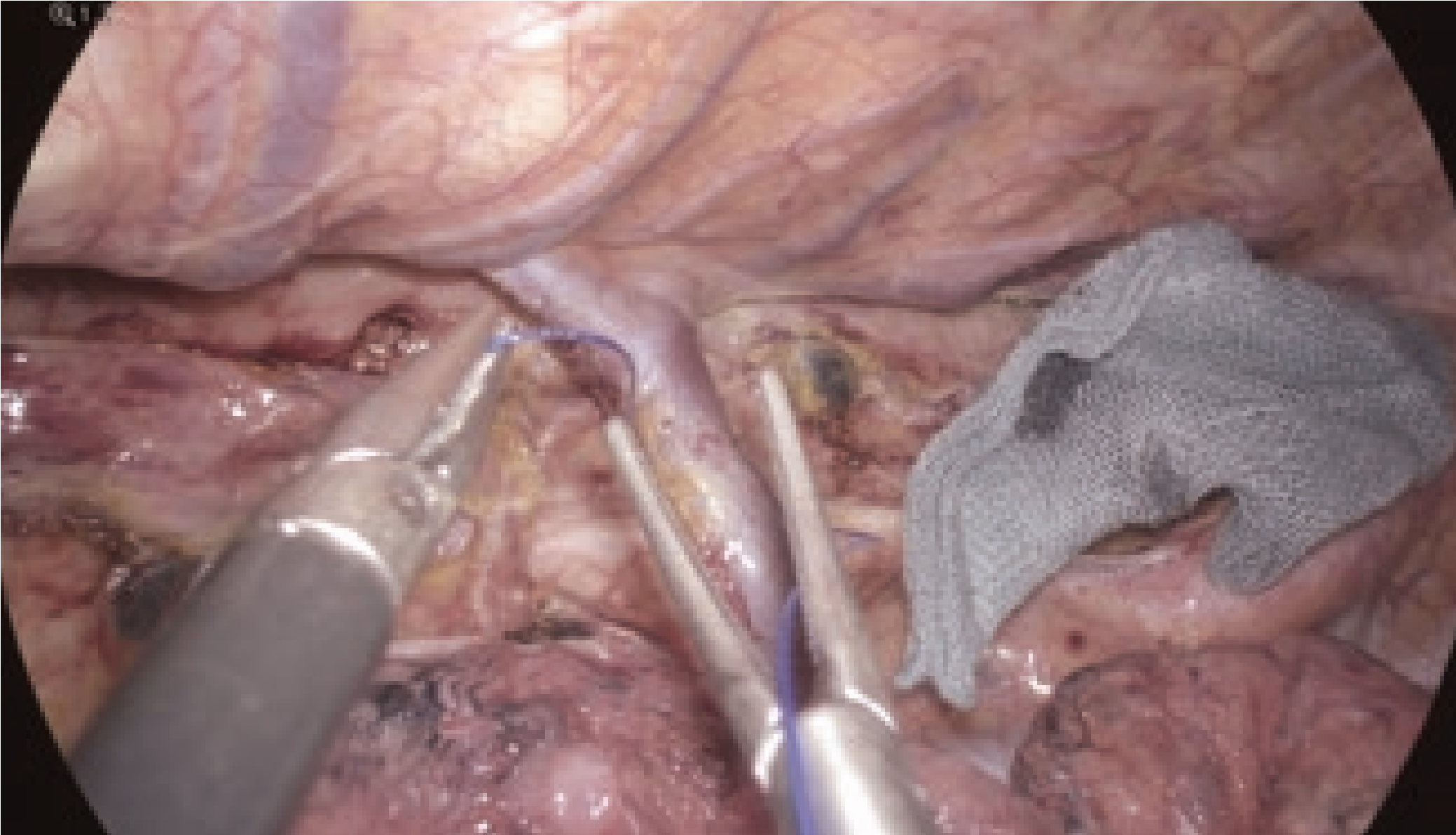
(stereoscopic vision)
2. Bleeding from small vessels
The high-definition image quality of the 4K endoscope allowed identification of a bleeding point, even from the small vessels.
Detailed observation of the hemorrhage also facilitated the selection of appropriate devices. Moreover, since clear images could be obtained during the zoom-in observation, the chance of fog accumulation on the lens was reduced, as was the frequency of cleaning the scope to remove dirt (e.g., mist). Attentive and meticulous surgery reduced bleeding and scope contamination, resulting in a dry and clear operative field.
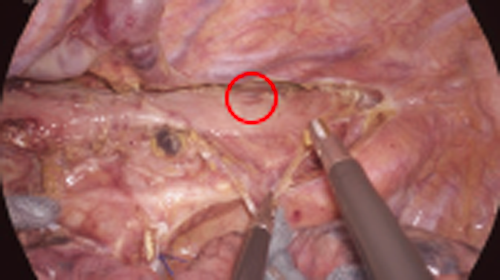
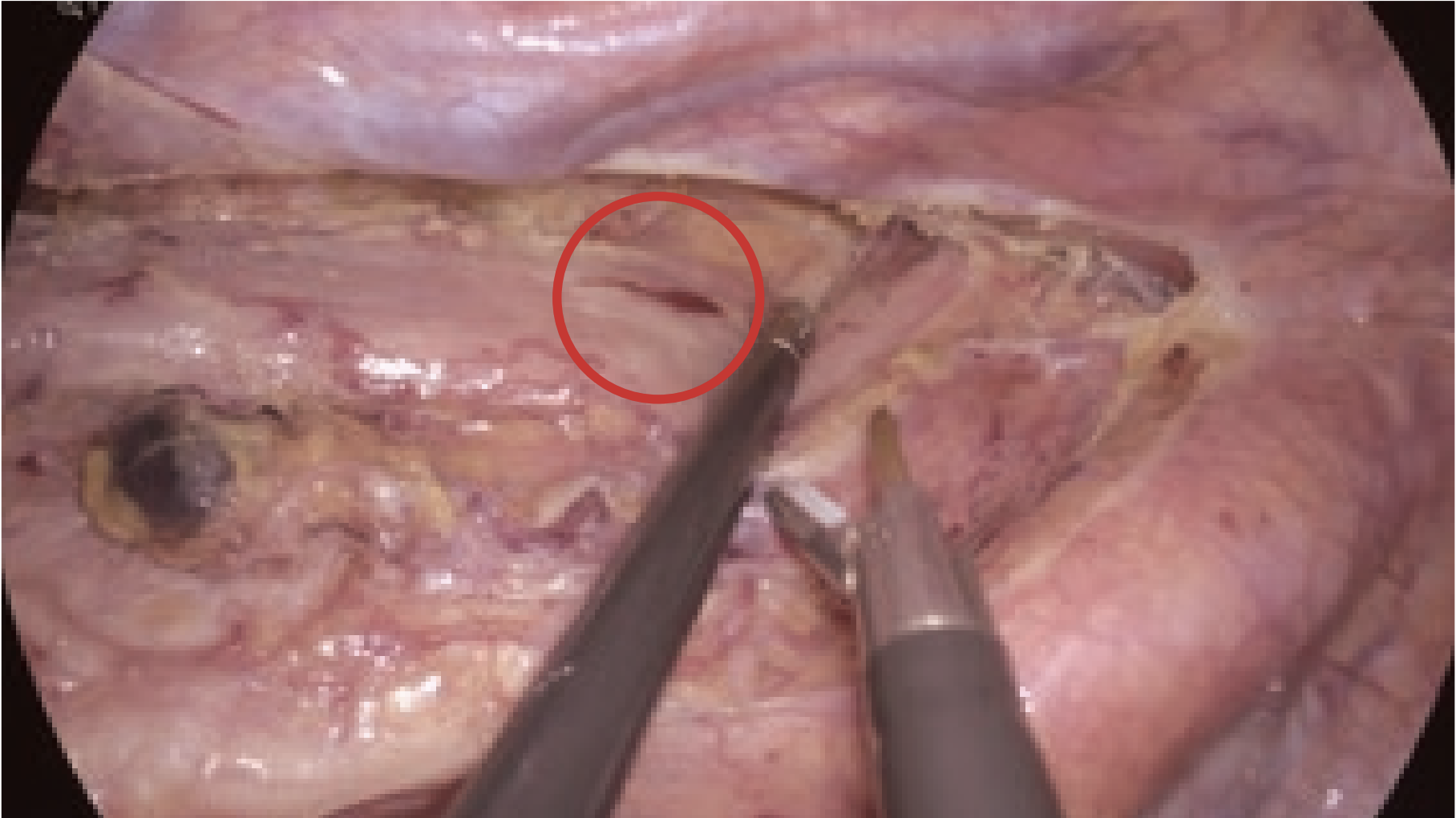
3. Identification of the right vagus nerve
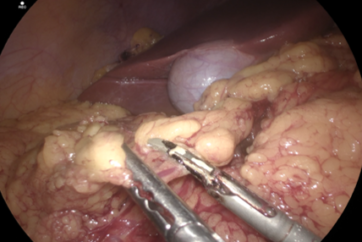
In identifying the right vagus nerve, the autofocus function and the electronic zoom magnification function allowed the easy focusing with minimal deterioration of image quality, resulting in the secure and delicate observation under magnification. If necessary, dissection could be performed using the THUNDERBEAT™ device. The 4K endoscope enabled observing the three pulmonary branches of the vagus nerve in the magnified image, which were otherwise difficult to visualize. After preservation, the esophagocardial branches were divided.
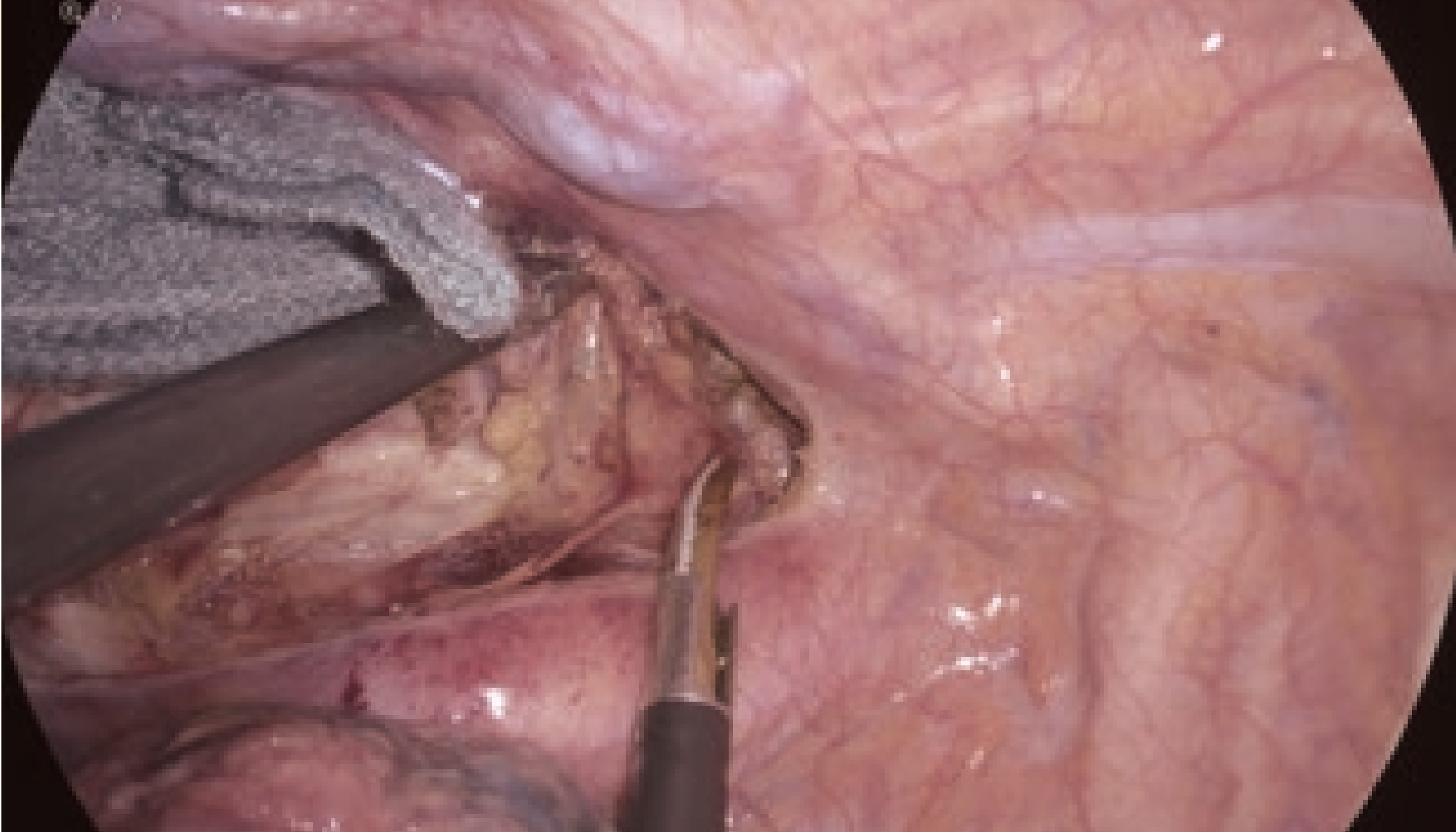
x 1.2
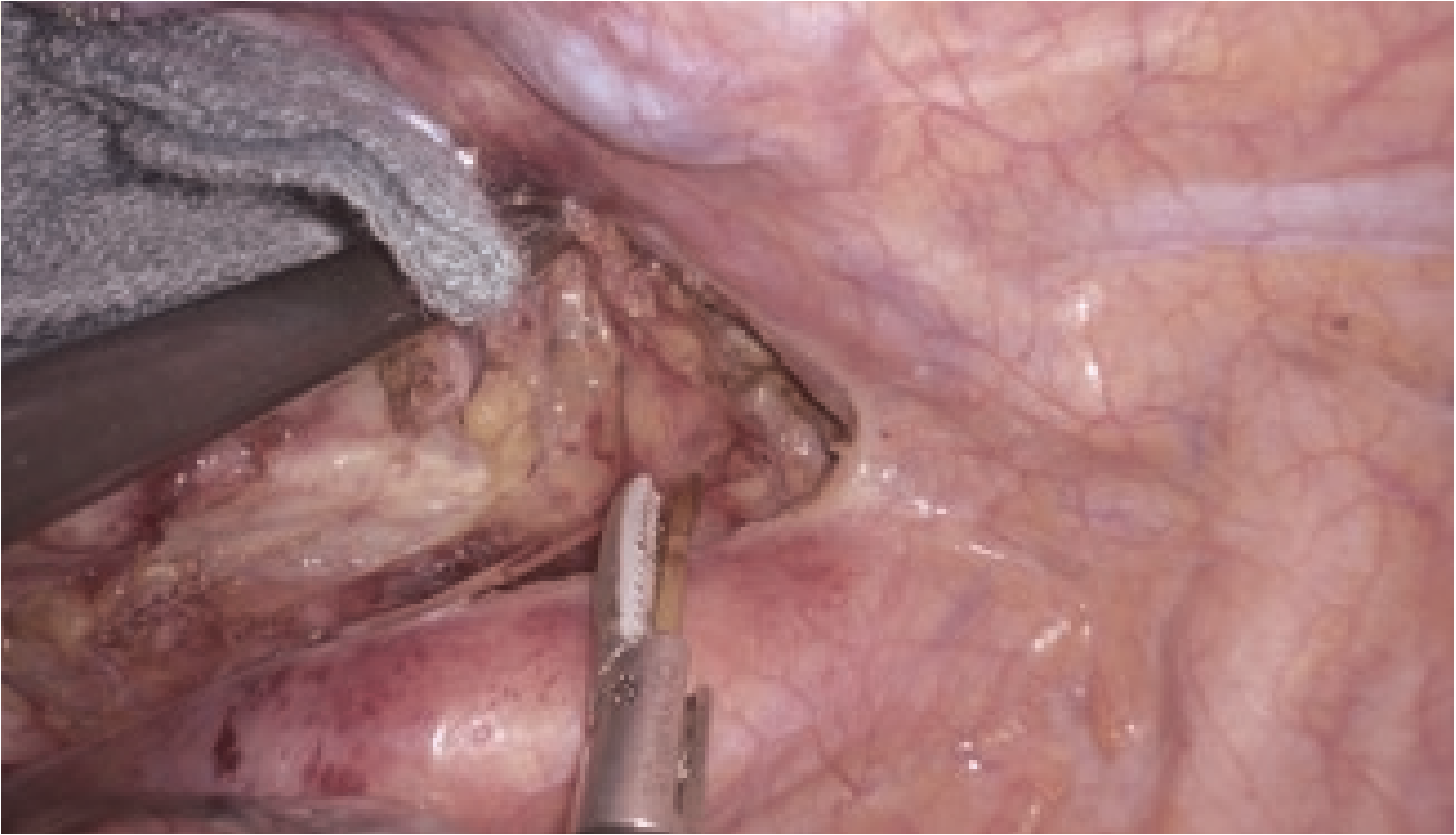
x 1.4
4. Manipulation within the right upper mediastinum
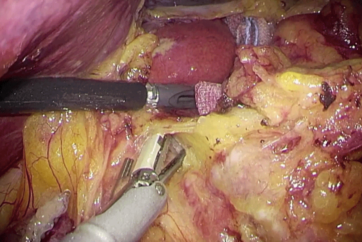
The right recurrent laryngeal nerve was identified. This nerve bifurcates from the right vagus nerve where the right subclavian artery originates from the brachiocephalic trunk, and winds behind the right subclavian artery.
The 4K endoscope experimentally used in the present case incorporated the BT2020 color gamut, the international standard, realizing a color gamut with an expressive capacity equivalent to 135% of the BT709 color gamut of the full HD endoscope. This provided accurate identification of nerves, vessels, muscle and fat tissue due to fractional image dissection in an objective manner.
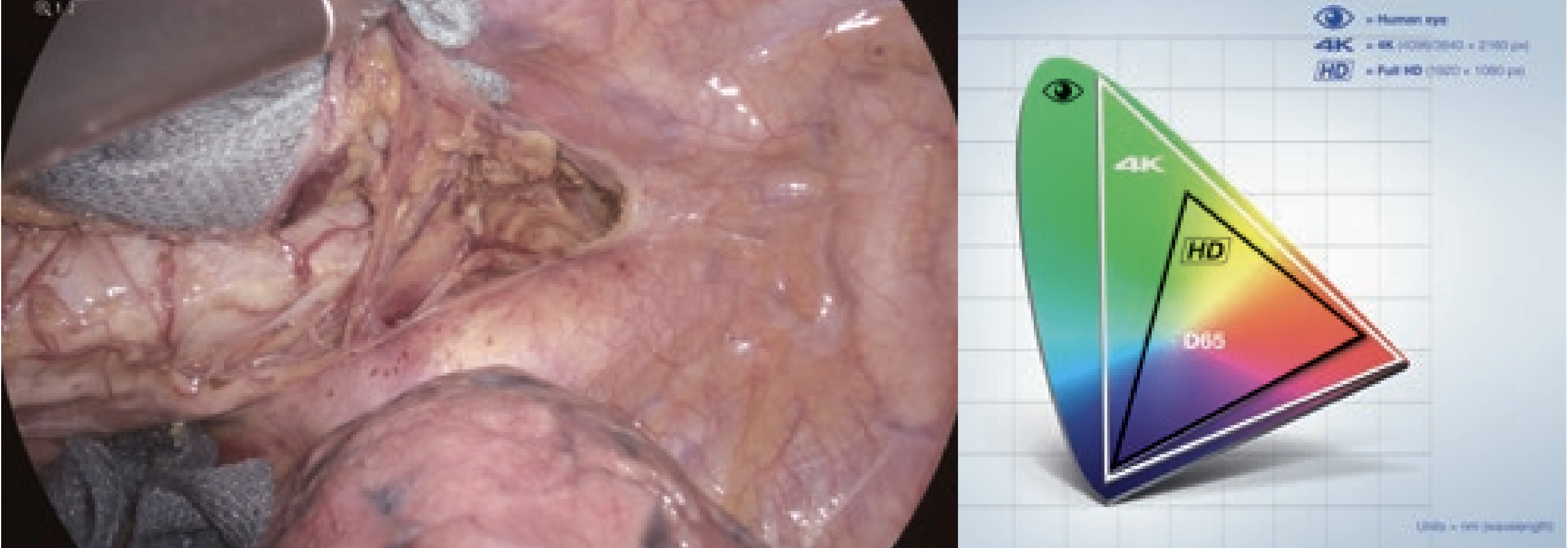
(wide color gamut)
5. Dissection of the lymph nodes from around the left recurrent laryngeal nerve to under the aortic arch
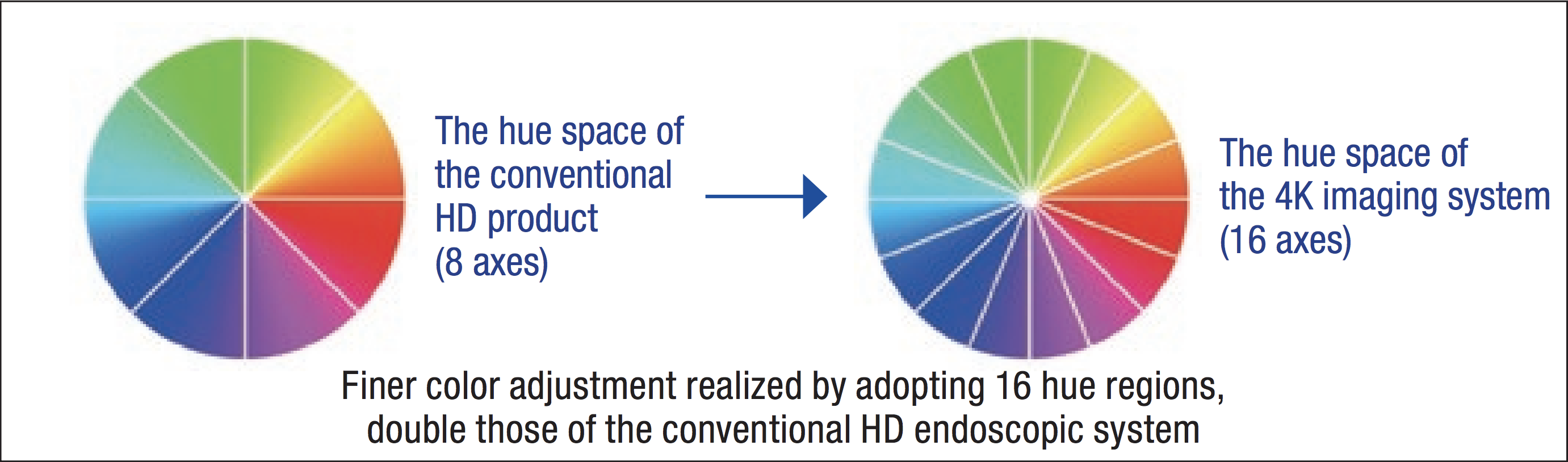
At the left face of the upper mediastinum, several cardiac branches of the sympathetic nervous system run parallel to the left recurrent laryngeal nerve. As these nerves are buried under the aorta and the sheaths of the left subclavian artery before entering the pericardium, only the fat tissue containing lymph nodes around the left recurrent laryngeal nerve was separated. In handling a complicated mutual transport network composed of the left recurrent laryngeal nerve and these cardiac branches of the sympathetic nerves, the visual field was maintained with a finely magnified observation image using the electronic magnification zoom. With the conventional full HD endoscope, it was sometimes difficult to differentiate tissues in the accumulated blood due to the flat color tones. The 4K endoscope provided for the differential resolution especially for red by adopting 16 hue regions, which is double that of a full HD endoscope. The use of this device during esophageal surgery is effective as it facilitated tissues discrimination in the accumulated blood.
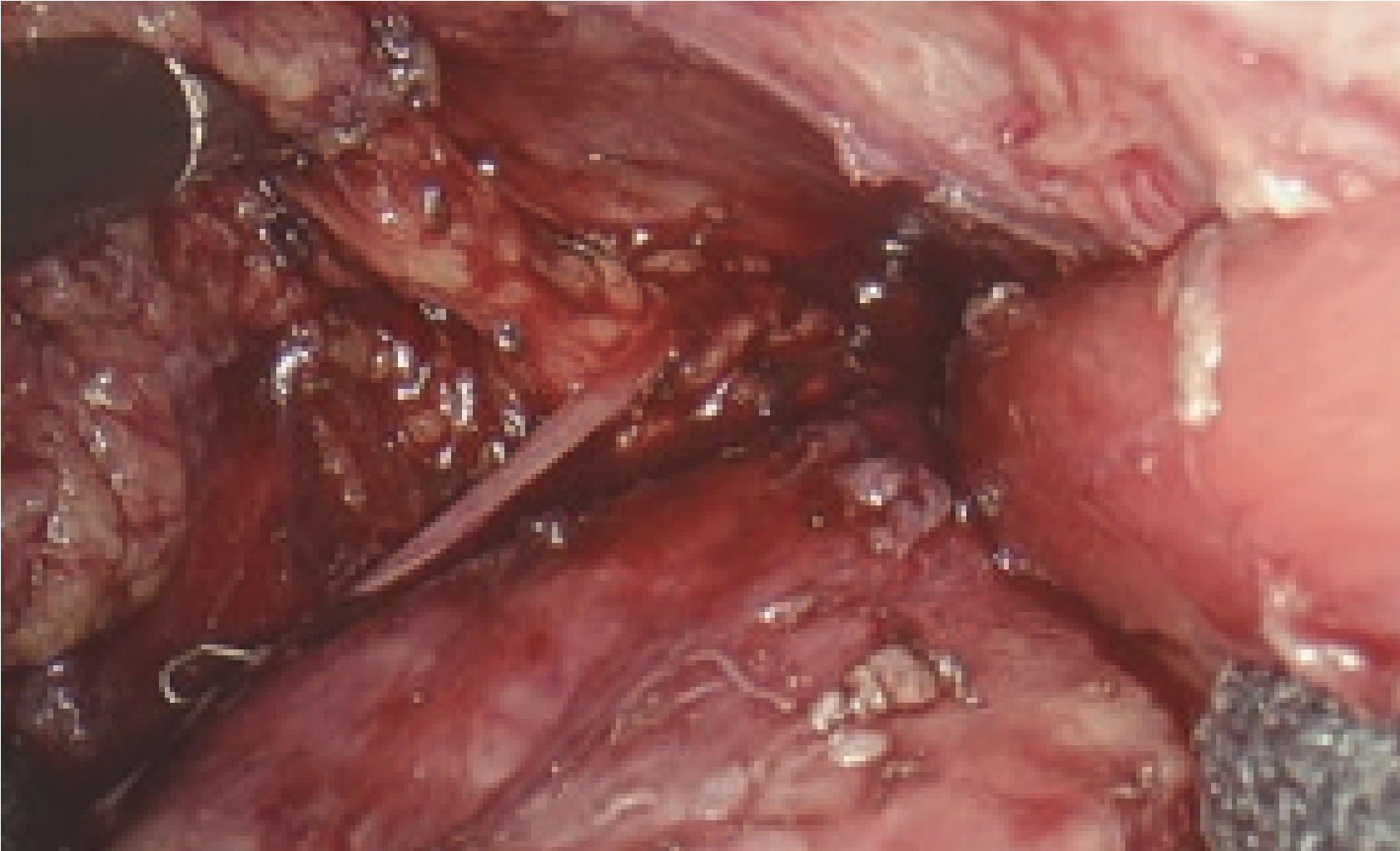
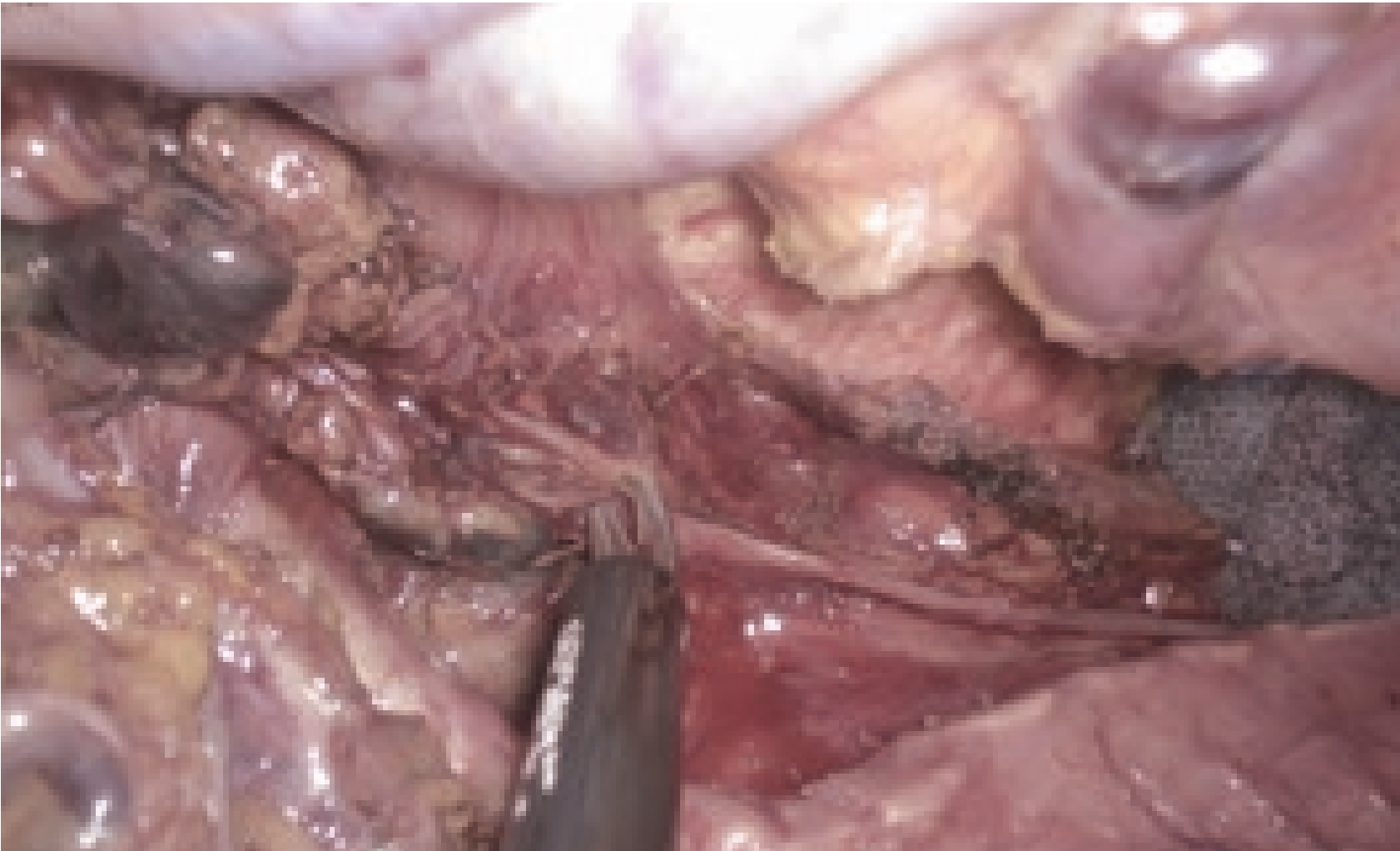
6. Sense of immersion provided by 4K/55-inch monitor and blue lamp
The 4K/55-inch monitor in front of the surgeon was a wide screen that covered the surgeon’s whole visual field and also provided the high-definition image quality of the 4K. Using this monitor together with the rendering LED lamp adopted at our hospital, we could focus intensely on the surgery with a sense of immersion as if we were operating inside of the thorax. Moreover, substantial educational advantages were anticipated, because the surgeon, assistant and camera assistant could share the microanatomy and tissue structures by viewing the 4K image on the monitor together.
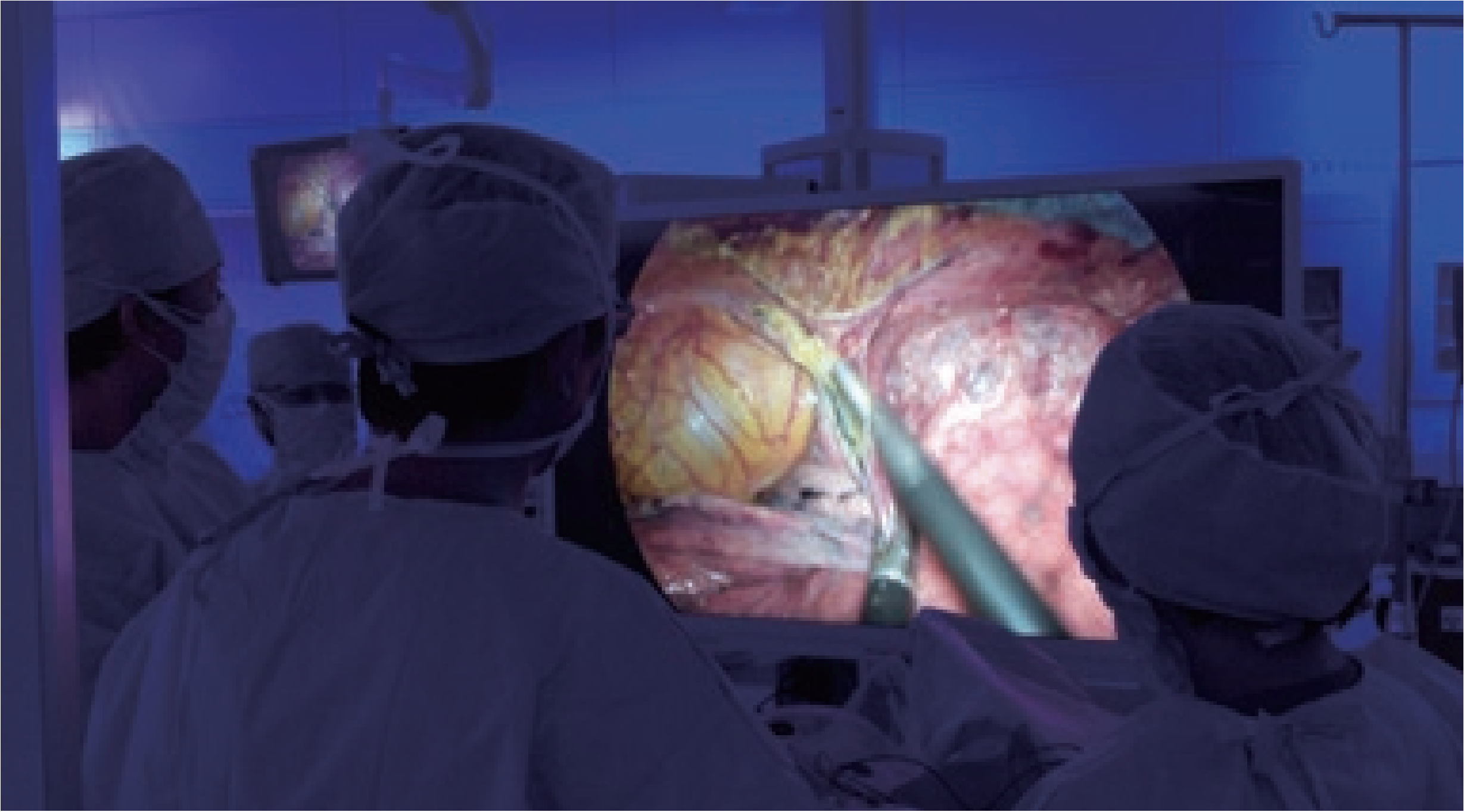
7. Summary
Meticulous and safe surgery could be performed comfortably using a dedicated endoscopy suite equipped with a high-resolution 4K endoscopic system, the 55-inch-wide monitor providing realistic visualization, high-performance devices and integration of individual devices.
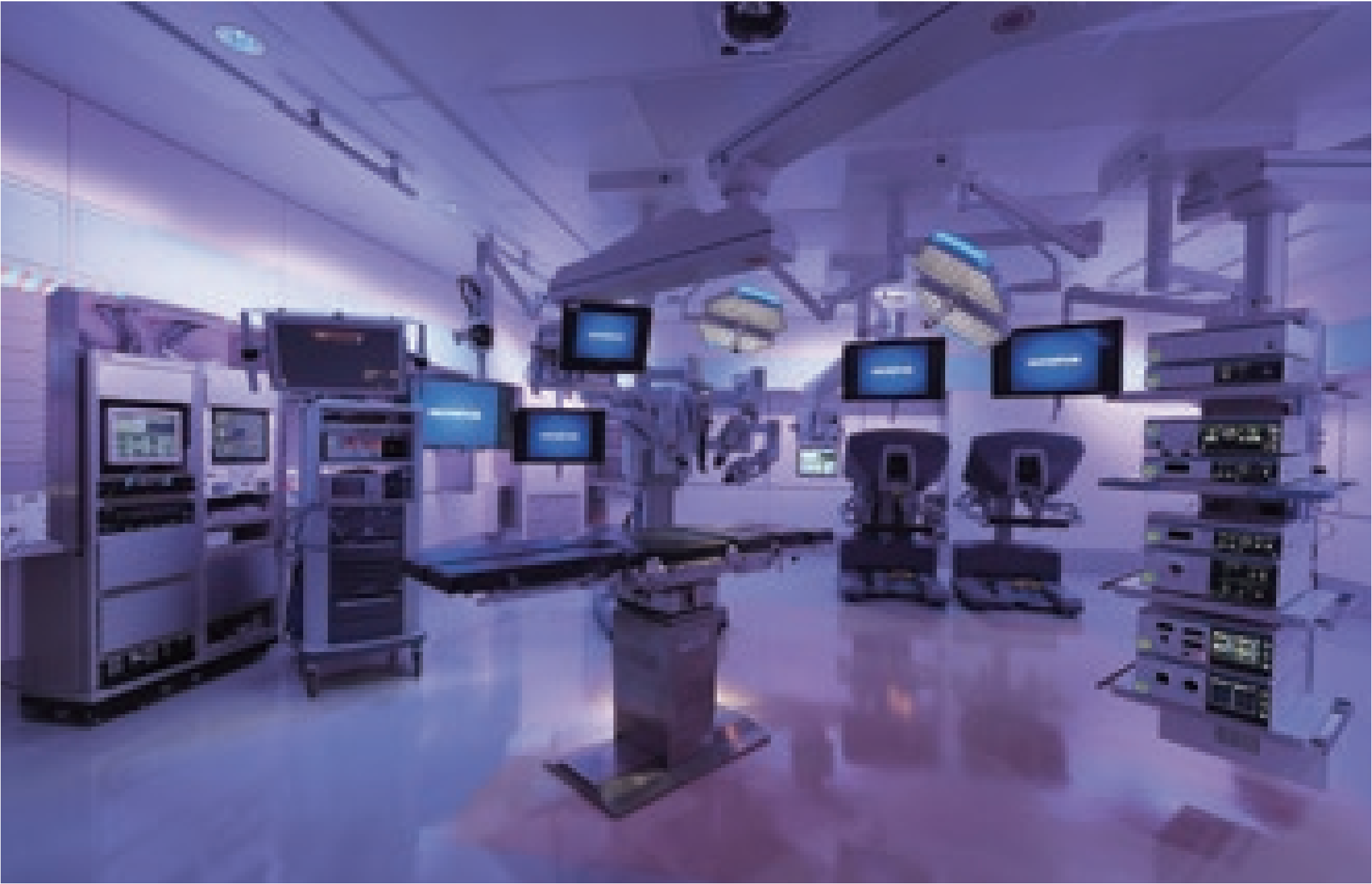
- Keyword
- Content Type