Cystoscopy at Samsung Medical Center

The number of cystoscopic procedures has significantly increased at Samsung Medical Center, Seoul, South Korea, following the purchase of 6 Olympus flexible cystoscopes in 2015.
We have interviewed Dr. Byong Chang Jeong, an Associate Professor in the Urology Department at Samsung Medical Center, for his commentary to hear the background of significant increase of cystoscopic procedures.
Doctor’s Biography
Byong Chang Jeong, M.D., Ph.D
Sungkyunkwan University School of Medicine, Seoul, South Korea
Samsung Medical Center, Seoul, South Korea
After graduating from the College of Medicine at Seoul National University (Seoul, South Korea) in 1996, Dr. Jung completed his residency, internship, and fellowship also at Seoul National University. He then worked as a urologist at the Armed Forces Capital Hospital (Seongnam, South Korea) and Seoul National University Hospital before assuming his current position of Associate Professor at the Department of Urology, Samsung Medical Center (Seoul, South Korea) in 2006. In 2012–2013, he completed a postdoctoral fellowship at Johns Hopkins Medical Institutions (Baltimore, Maryland, USA). Since 2014, he has assumed his current position of Associate Professor at the Department of Urology, Sungkyunkwan University School of Medicine (Seoul, South Korea).
Dr. Jeong is also a member of several professional societies including the Korean Urological Association, Korean Urological Oncology Society, Korean Endourology Society, and American Urological Association. He specializes in robotic operation, urological oncology (kidney, bladder, and prostate cancer), adrenal gland tumor, and benign prostate hyperplasia.
Cystoscopy at Samsung Medical Center
The most frequent indications for cystoscopy include visible hematuria and microscopic hematuria on laboratory examination, such as the occult blood test. Approximately 300–400 patients visit the Department of Urology, Samsung Medical Center, per day, which is the highest number of patients seen in South Korea.
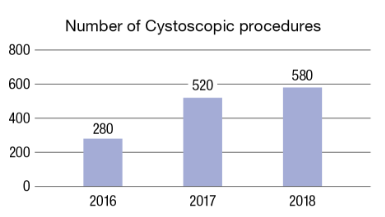
An average of 280 cystoscopic procedures/month was performed in 2016, 520 in 2017, and 580 in 2018 at Samsung Medical Center. Over this 3-year period, the mean number of patients who underwent cystoscopy was 460, and 350 (76%) patients were male. Among the 350 male patients, flexible cystoscopy was performed in 344 (98%) patients, whereas rigid cystoscopy was performed in only 6 (2%) patients. Due to the limited number of flexible cystoscope in the hospital, all female patients underwent rigid cystoscopy because the female urethra is much shorter than the male urethra and the procedure time is shorter in female patients than in male patients. However, there is no reason why flexible cystoscopy cannot be used in female patients. The current cystoscopy patient ratio of male:female is 3:1, however, Dr. Jeong believes that the proportion of female patients who undergo cystoscopy will increase by 20–30% if additional flexible cystoscopes are purchased and used for female patients.
| Rigid cystoscopy | Flexible cystoscopy | |
|---|---|---|
| Male (350) | 6 (2%) | 344 (98%) |
| Female (110) | 110 (100%) | 0 (0%) |
Frequencies of rigid and flexible cystoscopic procedures
performed by sex at Samsung Medical Center
Why flexible cystoscopy?
Less pain for patients
The primary advantage of flexible cystoscopy is that the patient experiences less pain during the procedure, especially for males since the male urethra is curved at an angle of nearly 90° and a rigid cystoscope causes severe pain when the cystoscope straightens the urethra to enter into the bladder. Rigid cystoscopy may also need to be performed under general anesthesia, whereas flexible cystoscopy merely requires local anesthesia.
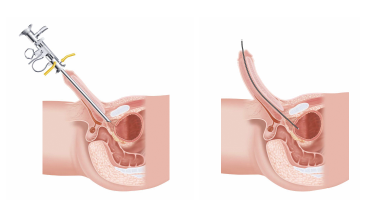
Even with flexible cystoscopes, the intensity of pain experienced by the patient is dependent on the shape of the tip of the scope, which can differ according to the manufacturer. CYF-VHA, a flexible cystoscope manufactured by Olympus, has a tapered tip called the “Evolution Tip” that may contribute to reduce the intensity of pain when the cystoscope is inserted into the urethra, prostate, and bladder.


The flexible cystoscope has possibility to reduce pain for the patient when the stent and Double-J catheter is inserted or removed. While rigid cystoscopy is easier to perform because the working channel for the rigid cystoscope is larger, the size of the rigid cystoscope is also much larger than the size of the flexible cystoscope (24 Fr. vs. 17 Fr., respectively). Therefore, the patient may feel less pain and be more comfortable while undergoing flexible cystoscopy. Dr. Jeong emphasized that “Double-J catheter removal is one of the greatest advantages about using the flexible cystoscope. Now my patients are very satisfied because the rigid cystoscope has been replaced with the flexible cystoscope.”
Another merit of the flexible cystoscope is that the outcome is not dependent on operator skill. Dr. Jeong states, “While I know how to prevent patients from feeling severe pain during rigid cystoscopy, only an experienced urologist can prevent it. By contrast, flexible cystoscopy can be performed without severe pain, even if it is performed by a resident who can only insert the polycatheter into the urethra.”
Patients undergoing flexible cystoscopy express greater satisfaction due to decreased pain and increased comfort as compared to rigid cystoscopy. Patients who come to Samsung Medical Center for cystoscopy often search online for information about the flexible cystoscope before their appointment and ask for the flexible cystoscope instead of the rigid cystoscope. Furthermore, individuals who undergo flexible cystoscopy after experiencing rigid cystoscopy never want to undergo rigid cystoscopy again. Many patients previously told Dr. Jeong, “I really want you to do my procedure, not other doctors” before flexible cystoscopy became available. This increase in patient satisfaction and comfort also seems to have had a direct effect on the number of flexible cystoscopic procedures performed, as the number of patients undergoing cystoscopy and patient revisit rates have increased after the introduction of flexible cystoscopy at Samsung Medical Center.
Better visibility of the bladder neck
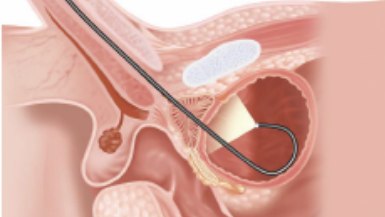
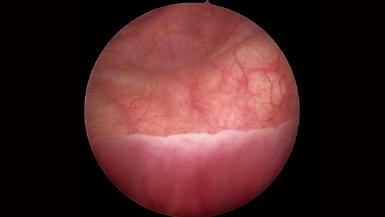
The second advantage of the flexible cystoscope is that the physician can clearly observe the area around the bladder neck and the blind spot by retroflexing the scope 180°. The field of view of the flexible cystoscope is quite different from that of the rigid cystoscope. The flexible cystoscope provides better visualization of all areas of the bladder than the rigid cystoscope because it has a wider deflection angle (30–110° vs. 70°, respectively). In particular, observation of the area around the bladder neck is very important, as lesions of the bladder neck are often missed especially in male patients. Moreover, in men with benign prostate hypertrophy (BPH), especially older men over 60s, there is a blind spot that is rarely seen in rigid cystoscopy that is visible in flexible cystoscopy.
Installation of the flexible cystoscope at Samsung Medical Center
Samsung Medical Center currently owns six Olympus flexible cystoscopes. Initially, Samsung Medical Center owned 3 flexible cystoscopes with poor image quality, therefore, they were rarely used. In 2015, Dr. Jeong met with Olympus and acquired the flexible cystoscope (CYF-VHA), which has superior image quality (high-definition) that is comparable with the rigid cystoscope. The CYF-VHA flexible cystoscope also has narrow band imaging (NBI) capability.
Considering patient satisfaction, Dr. Jeong started to persuade hospital management to procure an Olympus flexible cystoscope. This was not easy at first because the flexible cystoscope is more expensive than the rigid cystoscope and there is no difference in the insurance reimbursement fee between flexible and rigid cystoscopy in South Korea. Although the initial investment for flexible cystoscopy is costly, Dr. Jeong believed that the number of patients undergoing flexible cystoscopy would increase as patients prefer flexible cystoscopy, which is less painful than rigid cystoscopy. In fact, the number of cystoscopic procedures conducted at Samsung Medical Center significantly increased after purchasing the 6 Olympus flexible cystoscopes in 2015, which has allowed the institution to cover their initial investment. Dr. Jeong added, “A flexible cystoscope is one of the most effective items for bladder diagnosis. Approximately 460 cystoscopic
procedures are performed per month (about 20 procedures/day) at Samsung Medical Center. As each procedure takes up to 30 minutes to complete, approximately 14 cystoscopic procedures can be performed in one room per day.” Disinfection control is another important matter to consider. Prior to acquirement of a disinfection machine, only 3–4 of 6 flexible cystoscopes were available for cystoscopy due to time requirement for manual cleaning and disinfection. Samsung Medical Center purchased a disinfection machine for the 6 new flexible cystoscopes in 2017, and the number of flexible cystoscopic procedures greatly increased after the disinfection machine was installed.
Recommendations for flexible cystoscopy
Because the flexible cystoscope is easy to operate, even residents can easily learn how to use it after one or two attempts. Samsung Medical Center has a regular training program for residents. Video education is imparted twice a year, once in the first half of the year and once in the second half of the year. While bedside training is ideal, such training requires consent from patients, which is often difficult to obtain. Thus, training is conducted using dummy models. Dr. Jeong and other senior doctors used to perform all flexible cystoscopic procedures at Samsung Medical Center, but now the residents are capable of performing the procedure as well.
The angle of probe insertion is different between flexible and rigid cystoscopy. When performing rigid cystoscopy, the cystoscope is held in one hand and then pushed into the urethra. The cystoscope is then smoothed out from the point of entrapment at various angles to find a comfort zone for the patient. This is the part of the procedure when the patient experiences maximum pain and is especially painful in patients suffering from BPH. By contrast, in flexible cystoscopy, the cystoscope can be easily inserted with decreased angulation than the rigid cystoscope, which is more comfortable for the patient.
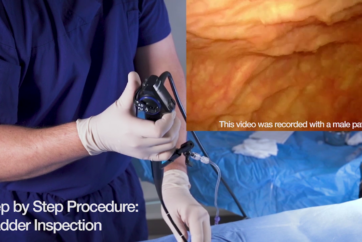
A physician who has just started to learn flexible cystoscopy should be well versed in the steps of flexible cystoscopy. This procedure is a step-by-step process that includes: (i) insertion, (ii) anterior urethra inspection including prostate inspection, (iii) bladder inspection, (iv) bladder neck inspection with NBI observation, and (v) scope retraction.
Conclusion
Dr. Jeong concluded that all cystoscopic procedures should be conducted using the flexible cystoscope and rigid cystoscopy should be used in very limited cases considering patient satisfaction and better observation of the bladder neck. Although the flexible cystoscope is generally more expensive than the rigid cystoscope, he is confident that the cost can be covered by the increasing number of patients who want to undergo flexible cystoscopy. Dr. Jeong also mentioned that he would like his institution to acquire additional flexible cystoscopes to perform flexible cystoscopy for female patients as well.
- Keyword
- Content Type